Urology — MCQs

On this page
Normal urine flow rate in healthy adults in urodynamic study is -
Radical nephrectomy involves resection of the following structures, which one is not typically resected?
What is the most common site of penile carcinoma?
A 40-year-old male presents with translucent scrotal swelling in which it is possible to get above the swelling on examination. What is the most probable diagnosis?
What is the main hazard of ectopic testis -
Which type of renal stone is known to have less satisfactory results with extracorporeal shock wave lithotripsy (ESWL)?
What is the most appropriate treatment for a patient with symptomatic bladder stones?
At what age is orchidopexy for an incompletely descended testis typically performed?
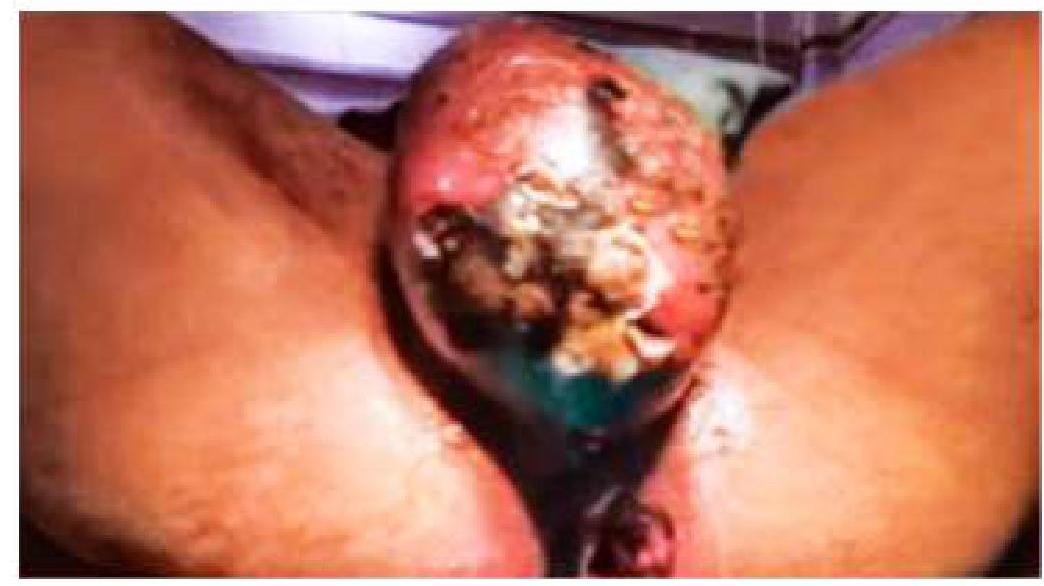
An elderly male patient presented with a sudden onset of scrotal pain and discharge as shown in the image. What is the likely diagnosis?
Treatment of Renal cell carcinoma of less than 4 cm will be?
Urology Indian Medical PG Practice Questions and MCQs
Question 1001: Normal urine flow rate in healthy adults in urodynamic study is -
- A. 10 ml/sec
- B. 5 ml/sec
- C. 20 ml/sec (Correct Answer)
- D. 25 ml/sec
Explanation: ***20 ml/sec*** - A peak urinary flow rate of **20 mL/second** is considered normal in healthy adult males when voiding a volume of 200 mL or more. - In women, a maximum flow rate above **25 mL/second** is considered normal when voiding similar volumes. *10 ml/sec* - A maximum flow rate of less than **15 mL/second** is commonly considered to suggest significant bladder outlet obstruction in men. - This value is generally indicative of a potentially abnormal urinary flow, requiring further investigation. *25 ml/sec* - While **25 mL/second** or more is considered normal for women, for men, this rate is at the higher end of the normal range and not the average healthy adult flow rate. - This option is more typically associated with unimpeded flow in females, not the general population of healthy adults. *5 ml/sec* - A flow rate of **5 mL/second** is significantly below the normal range for healthy adults and would suggest a severe urinary obstruction or very poor detrusor function. - This value is usually seen in patients with significant bladder outlet obstruction or compromised bladder muscle function.
Question 1002: Radical nephrectomy involves resection of the following structures, which one is not typically resected?
- A. Gerota's fascia
- B. Surrounding hilar lymph nodes
- C. Proximal para-aortic lymph nodes (Correct Answer)
- D. Ipsilateral adrenal gland (in classical approach)
Explanation: ***Proximal para-aortic lymph nodes*** - **Proximal para-aortic lymph nodes** are NOT routinely resected during radical nephrectomy unless there is evidence of gross nodal involvement on imaging or intraoperatively. - The extent of lymph node dissection is tailored to individual disease burden; hilar and regional nodes are addressed, but distant nodal groups like proximal para-aortic nodes are only resected when clearly involved. - Extended lymphadenectomy to proximal para-aortic regions is not part of standard radical nephrectomy. *Gerota's fascia* - **Gerota's fascia** (perirenal fascia) is **always resected** in radical nephrectomy as it encases the kidney and perirenal fat. - En bloc resection of Gerota's fascia with the kidney ensures complete tumor removal, clear margins, and prevents tumor spillage. - This is a defining component of "radical" versus "simple" nephrectomy. *Ipsilateral adrenal gland (in classical approach)* - In **classical radical nephrectomy** (Campbell-Walsh traditional description), the ipsilateral adrenal gland was routinely removed due to proximity and concern for tumor extension. - **Modern practice** has shifted to adrenal-sparing nephrectomy as the standard, with adrenalectomy reserved for upper pole tumors with direct invasion, bulky tumors, or imaging abnormalities. - For this question's context of "classical radical nephrectomy," the adrenal gland **IS typically resected** in the traditional approach. *Surrounding hilar lymph nodes* - **Hilar lymph nodes** are routinely resected during radical nephrectomy for staging and regional disease control. - These nodes are the first-line lymphatic drainage sites and their removal is integral to proper oncologic surgery. - Hilar lymphadenectomy is a standard component of radical nephrectomy.
Question 1003: What is the most common site of penile carcinoma?
- A. Glans (Correct Answer)
- B. Prepuce
- C. Shaft
- D. Coronal sulcus
Explanation: ***Glans*** - The **glans penis** is the most frequent site of origin for penile carcinoma due to its exposure and susceptibility to chronic irritation and inflammation. - Approximately **50-70%** of penile cancers originate on the glans. *Prepuce* - The **prepuce** (foreskin) is the second most common site, often affected in uncircumcised males, but less frequently than the glans itself. - Carcinomas here often develop at the **mucocutaneous junction** of the prepuce. *Shaft* - The **penile shaft** is a much less common site for penile carcinoma, accounting for a smaller percentage of cases. - Cancers on the shaft tend to be **more aggressive** and may present with different clinical features. *Coronal sulcus* - The **coronal sulcus** is the groove between the glans and the shaft. While it's a common site for lesions, it is still less common than the glans itself for the primary origin of carcinoma. - Lesions here can often spread to the glans or prepuce, making the distinction difficult without a clear point of origin.
Question 1004: A 40-year-old male presents with translucent scrotal swelling in which it is possible to get above the swelling on examination. What is the most probable diagnosis?
- A. Hydrocele (Correct Answer)
- B. Indirect inguinal hernia
- C. Varicocele
- D. Sebaceous cyst
Explanation: ***Hydrocele*** - A **hydrocele** is characterized by a translucent scrotal swelling because it contains **serous fluid**, allowing light to pass through. - The ability to **get above the swelling** on examination indicates that it is confined to the scrotum and not extending into the inguinal canal, differentiating it from an indirect inguinal hernia. *Indirect inguinal hernia* - An **indirect inguinal hernia** is a protrusion of abdominal contents through the deep inguinal ring into the scrotum, meaning it would **not be possible to get above the swelling**. - It would typically be **non-translucent** as it contains bowel or omentum, not serous fluid. *Varicocele* - A **varicocele** is a collection of dilated veins in the pampiniform plexus, often described as a **"bag of worms"** on palpation, and is typically not translucent. - While located in the scrotum, it is usually distinguishable by its **palpable vascular nature** and often changes with Valsalva maneuver. *Sebaceous cyst* - A **sebaceous cyst** is a benign growth filled with keratinous material, originating from a blocked sebaceous gland. - It would be a **firm, non-translucent lump** and not a generalized scrotal swelling that allows light transmission.
Question 1005: What is the main hazard of ectopic testis -
- A. Risk of carcinoma development (Correct Answer)
- B. Increased risk of impotence
- C. Risk of hernia development
- D. Liable to injury
Explanation: ***Risk of carcinoma development*** - Ectopic testis, like undescended testis (cryptorchidism), carries an **increased risk of germ cell tumors**, particularly **seminoma**. - An **ectopic testis** is one that has descended but deviated from the normal path and is located in an abnormal position (superficial inguinal pouch, perineum, femoral triangle, etc.). - While the malignancy risk in ectopic testis may be **slightly lower than true cryptorchidism**, it remains the **most significant long-term hazard**. - The increased risk is attributed to **abnormal testicular development** and **dysgenesis**, leading to potential malignant transformation. - Risk is estimated at **4-10 times higher** than normally descended testes. *Increased risk of impotence* - Ectopic testes can affect **fertility** due to impaired spermatogenesis from abnormal positioning and higher temperatures. - However, they do **not directly cause impotence** (erectile dysfunction). - Impotence relates to inability to achieve or maintain erection, which is a vascular, neurological, or psychological issue, not affected by testicular position. *Risk of hernia development* - An **inguinal hernia** can be associated with undescended testis if the processus vaginalis remains patent. - An ectopic testis, having deviated outside the normal path of descent, does **not typically predispose to hernia** formation in the same manner. - This is not the primary concern with ectopic testis. *Liable to injury* - An ectopic testis located in superficial positions (superficial inguinal pouch, perineum) is **more vulnerable to trauma** than a normally descended scrotal testis. - While trauma risk is a legitimate concern, it is **secondary** to the long-term risk of **malignancy**. - The risk of cancer development far outweighs the risk of traumatic injury in clinical significance.
Question 1006: Which type of renal stone is known to have less satisfactory results with extracorporeal shock wave lithotripsy (ESWL)?
- A. Oxalate stone
- B. Phosphate stone
- C. Urate stone
- D. Cystine stone (Correct Answer)
Explanation: ***Cystine stone*** - **Cystine stones** are known for their high **elasticity** and durable molecular bonds, making them resistant to fragmentation by **extracorporeal shock wave lithotripsy (ESWL)**. - Their physical properties result in **less satisfactory fragmentation rates** compared to other stone types, often requiring multiple ESWL sessions or alternative treatments. *Oxalate stone* - **Calcium oxalate stones** are generally **amenable to ESWL**, especially smaller ones, as they tend to fragment well. - They are the **most common type of kidney stone**, and ESWL is a primary treatment modality for many of these. *Phosphate stone* - **Calcium phosphate stones** (e.g., brushite, apatite) and **struvite stones** also tend to respond reasonably well to ESWL. - While sometimes harder than oxalate stones, they usually **fragment effectively** with shock waves. *Urate stone* - **Uric acid stones** are typically **radiolucent** but generally respond well to ESWL, often fragmenting into small pieces. - They can also be dissolved with **urinary alkalinization**, which is a unique therapeutic option for this stone type.
Question 1007: What is the most appropriate treatment for a patient with symptomatic bladder stones?
- A. Transurethral litholapaxy (Correct Answer)
- B. Percutaneous suprapubic litholapaxy
- C. Vesicotomy and stone retrieval
- D. Intravenous antibiotics
Explanation: ***Transurethral litholapaxy*** - This procedure involves inserting a **cystoscope** through the urethra into the bladder to visualize and then fragment the stone using various energy sources (e.g., laser, pneumatic, ultrasound). - The fragmented pieces are then irrigated and removed, offering a **minimally invasive** and highly effective treatment for most bladder stones. *Percutaneous suprapubic litholapaxy* - This method is typically reserved for very **large or complex bladder stones** that are difficult to manage transurethrally. - It involves accessing the bladder directly through a **suprapubic incision**, which is more invasive than the transurethral approach. *Vesicotomy and stone retrieval* - A **vesicotomy** (open surgical incision into the bladder) is a more invasive procedure, usually considered when other less invasive methods have failed or are not feasible. - This approach carries higher risks, including **longer recovery times** and potential for greater complications compared to endoscopic options. *Intravenous antibiotics* - **Antibiotics** are used to treat or prevent urinary tract infections that may be associated with bladder stones, but they do not remove or dissolve the stones themselves. - While infection may be a concurrent issue, antibiotics alone **do not address the physical obstruction** or symptomatic cause of bladder stones.
Question 1008: At what age is orchidopexy for an incompletely descended testis typically performed?
- A. At birth
- B. 1 year (Correct Answer)
- C. 2 years
- D. 5 years
Explanation: ***1 year*** - Orchidopexy is typically recommended between **6 and 12 months** of age to prevent long-term complications like **infertility** and **malignancy**. - Performing the surgery at this age maximizes the chances of **normal testicular development** and reduces the risk of germ cell destruction. *At birth* - It is generally not performed at birth because **spontaneous descent** can still occur within the first few months of life. - Early intervention is usually reserved for specific conditions like **testicular torsion**. *2 years* - Waiting until 2 years of age is considered **too late**, as prolonged exposure to higher abdominal temperatures can cause **irreversible damage** to the testicular tissue. - This delay increases the risk of **compromised fertility** and a higher incidence of **testicular cancer**. *5 years* - Performing orchidopexy at 5 years is significantly **too late**, leading to a high risk of **infertility** and a severely increased risk of **testicular cancer**. - By this age, the potential for normal testicular development is greatly diminished.
Question 1009: An elderly male patient presented with a sudden onset of scrotal pain and discharge as shown in the image. What is the likely diagnosis?
- A. Fournier’s gangrene (Correct Answer)
- B. Torsion of testis
- C. Scrotal carcinoma
- D. Acute epididymo-orchitis
Explanation: ***Fournier's gangrene*** - The sudden onset of scrotal pain with discharge in an elderly male, combined with **tissue necrosis** and extensive scrotal skin changes, is characteristic of **Fournier's gangrene** (necrotizing fasciitis of the genitalia). - Elderly males are at higher risk due to **diabetes**, **immunocompromise**, and **urogenital infections**, making this a rapidly progressive and potentially life-threatening condition requiring urgent surgical debridement. *Acute epididymo-orchitis* - While epididymo-orchitis can cause scrotal pain and discharge, it typically does **not cause tissue necrosis** or the extensive scrotal skin changes described. - It presents as **localized inflammation** of the epididymis/testis without the widespread necrotizing changes seen in this case. *Torsion of testis* - Testicular torsion typically presents with **abrupt, severe scrotal pain** and swelling, but usually **without discharge** or the extensive scrotal skin changes seen here. - It constitutes a **surgical emergency** due to compromised blood supply to the testis, but doesn't involve necrotizing infection. *Scrotal carcinoma* - Scrotal carcinoma usually presents as a **painless mass or ulceration** that grows over time, rather than a sudden onset of severe pain and discharge. - It represents a **chronic process** and doesn't typically cause the acute necrotizing inflammatory changes observed in this case.
Question 1010: Treatment of Renal cell carcinoma of less than 4 cm will be?
- A. Radical nephrectomy
- B. Radical nephrectomy + postoperative radiotherapy
- C. Radical nephrectomy + chemotherapy
- D. Partial nephrectomy (Correct Answer)
Explanation: ***Partial nephrectomy*** - For **renal cell carcinoma (RCC) less than 4 cm** (T1a tumors), **partial nephrectomy** is the preferred treatment. This approach aims to preserve as much healthy renal tissue as possible, reducing the risk of chronic kidney disease, especially in patients with normal contralateral kidneys. - Studies have shown that partial nephrectomy offers comparable **oncologic outcomes** to radical nephrectomy for small tumors while providing better overall kidney function. *Radical nephrectomy* - While effective for larger tumors or those invading surrounding structures, **radical nephrectomy** involves removing the entire kidney, which may lead to a higher risk of **chronic kidney disease** compared to partial nephrectomy for small tumors. - This option is generally reserved for **larger tumors** (T1b or greater), more complex cases, or when partial nephrectomy is not feasible due to tumor location or patient comorbidities. *Radical nephrectomy + postoperative radiotherapy* - **Radiotherapy** is generally not effective in treating renal cell carcinoma (RCC) due to the **radioresistant nature** of the tumor cells. It is rarely used in the primary treatment of RCC. - The combination of radical nephrectomy and postoperative radiotherapy would expose the patient to unnecessary treatment with significant side effects without clear survival benefits for localized disease. *Radical nephrectomy + chemotherapy* - **Chemotherapy** has historically shown **limited efficacy** in the treatment of renal cell carcinoma, particularly for localized disease. It is primarily used in advanced, metastatic RCC, and newer targeted therapies and immunotherapies are often preferred. - For small, localized tumors, surgery alone is curative, and adding chemotherapy to radical nephrectomy would introduce **unnecessary toxicity** without improving outcomes.
Practice by Chapter
Urological Anatomy
Practice Questions
Hematuria Evaluation
Practice Questions
Urinary Calculi
Practice Questions
Benign Prostatic Hyperplasia
Practice Questions
Prostate Cancer
Practice Questions
Bladder Cancer
Practice Questions
Renal Cell Carcinoma
Practice Questions
Testicular Tumors
Practice Questions
Urinary Tract Infections
Practice Questions
Urinary Incontinence
Practice Questions
Genitourinary Trauma
Practice Questions
Pediatric Urology Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Start For Free