Internal Medicine
1 questionsWireless capsule endoscopy is done to visualize which of the following condition?
NEET-PG 2013 - Internal Medicine NEET-PG Practice Questions and MCQs
Question 1281: Wireless capsule endoscopy is done to visualize which of the following condition?
- A. Esophageal varices
- B. Gastric carcinoma
- C. Crohn's disease (Correct Answer)
- D. Ulcerative colitis
Explanation: ***Crohn's disease*** - Wireless capsule endoscopy is primarily used to visualize the **small bowel**, which is the main site of involvement in Crohn's disease [3]. - It helps detect **mucosal inflammation**, ulcers, and strictures that may not be accessible by conventional endoscopy [1]. *Esophageal varices* - **Esophageal varices** are best visualized and treated with conventional **esophagogastroduodenoscopy (EGD)**, which allows for direct intervention [2]. - Capsule endoscopy is not the preferred method due to its inability to adequately distend the esophagus or perform therapeutic maneuvers [4]. *Gastric carcinoma* - Diagnosing **gastric carcinoma** requires visualization of the stomach lining, typically achieved through **conventional upper endoscopy** with biopsies [2]. - The capsule may pass too quickly through the stomach or miss subtle lesions, and it cannot obtain tissue samples. *Ulcerative colitis* - **Ulcerative colitis** primarily affects the **colon**, which is visualized using a **colonoscopy** [3]. - While capsule endoscopy can visualize the small bowel, it is not effective for examining the colon due to insufficient imaging of the entire large intestine and lack of biopsy capabilities.
Obstetrics and Gynecology
3 questionsWhat is the recommended timing for the insertion of a Copper T intrauterine device?
Most common congenital uterine anomaly is?
Which drug is commonly used in the medical management of ectopic pregnancy?
NEET-PG 2013 - Obstetrics and Gynecology NEET-PG Practice Questions and MCQs
Question 1281: What is the recommended timing for the insertion of a Copper T intrauterine device?
- A. 3 days after periods are over
- B. Within 10 days of start of menstrual cycle (Correct Answer)
- C. Just after menstruation
- D. During active pelvic infection
Explanation: ***Within 10 days of start of menstrual cycle*** - Inserting the **Copper T IUD** during this phase ensures the woman is not pregnant, as ovulation typically occurs later in the cycle. - The **cervix is slightly dilated** during menstruation, making insertion easier and less uncomfortable. - This is the **recommended timing** as per standard guidelines for IUD insertion. *3 days after periods are over* - While this timing might seem appropriate, it doesn't align with the optimal window for ensuring **non-pregnancy** and ease of insertion. - The **cervix may have already closed** significantly, making insertion potentially more difficult than during menstruation. *During active pelvic infection* - Insertion of an IUD during an **active pelvic infection** is **absolutely contraindicated** due to the risk of exacerbating the infection and leading to more serious complications like **pelvic inflammatory disease (PID)**. - The presence of infection increases the likelihood of bacteria being carried into the **uterine cavity**, potentially causing severe consequences. *Just after menstruation* - While close to the ideal window, this timing is less specific than "within 10 days" and may miss the optimal cervical conditions. - The benefits of a slightly dilated cervix during the early menstrual phase would be maximized with the more precise timing of within 10 days of cycle start.
Question 1282: Most common congenital uterine anomaly is?
- A. Bicornuate uterus
- B. Unicornuate uterus
- C. Arcuate uterus
- D. Septate uterus (Correct Answer)
Explanation: ***Septate uterus*** - A septate uterus is the most common congenital uterine anomaly, characterized by a **fibrous or muscular septum** dividing the uterine cavity. - This anomaly results from incomplete resorption of the **müllerian ducts** during development. *Bicornuate uterus* - A bicornuate uterus involves **two uterine horns** that are partially or completely separate, leading to a heart-shaped uterus. - While relatively common, it is **less prevalent** than the septate uterus. *Unicornuate uterus* - A unicornuate uterus is an anomaly where only **one side of the müllerian duct develops**, resulting in a uterus with only one horn and one fallopian tube. - This is a **rare anomaly** compared to septate and bicornuate uteri. *Arcuate uterus* - An arcuate uterus is considered a **mild variant of a normal uterus**, with a slight indentation in the fundus. - It often has **no clinical significance** and is less severe than other anomalies.
Question 1283: Which drug is commonly used in the medical management of ectopic pregnancy?
- A. Leuprolide
- B. Methotrexate (Correct Answer)
- C. Mifepristone
- D. Carboprost
Explanation: ***Correct: Methotrexate*** - **Methotrexate** is a **folic acid antagonist** that inhibits DNA synthesis and cell proliferation, making it effective in terminating early ectopic pregnancies by targeting rapidly dividing trophoblastic cells. - It is typically considered for **hemodynamically stable** patients with unruptured ectopic pregnancies, a beta-hCG level below a certain threshold (e.g., <5,000 mIU/mL), and no cardiac activity in the ectopic mass. - This is the **gold standard** for medical management of ectopic pregnancy meeting specific criteria. *Incorrect: Mifepristone* - **Mifepristone** is an **antiprogestin** primarily used for medical abortion of intrauterine pregnancies, causing detachment of the gestational sac and cervical ripening. - While it can be used in combination with misoprostol for medical abortion, it is **not the primary drug** for managing ectopic pregnancies. *Incorrect: Leuprolide* - **Leuprolide** is a **GnRH agonist** mainly used for conditions like endometriosis, uterine fibroids, and prostate cancer by suppressing ovarian or testicular hormone production. - It is **not used** in the direct medical management of ectopic pregnancy. *Incorrect: Carboprost* - **Carboprost** is a **prostaglandin F2-alpha analog** primarily used to treat **postpartum hemorrhage** by inducing strong uterine contractions. - It is **not indicated** for the treatment of ectopic pregnancy.
Ophthalmology
1 questionsFluorescein angiography is used to examine -
NEET-PG 2013 - Ophthalmology NEET-PG Practice Questions and MCQs
Question 1281: Fluorescein angiography is used to examine -
- A. Ciliary vasculature
- B. Retinal vasculature (Correct Answer)
- C. Corneal vasculature
- D. Conjunctival vasculature
Explanation: ***Retinal vasculature*** - **Fluorescein angiography** involves injecting fluorescein dye into a vein and taking rapid photographs of the retina as the dye perfuses, allowing for detailed visualization of the **retinal blood vessels**. - This technique is crucial for diagnosing and monitoring conditions like **diabetic retinopathy**, **macular degeneration**, and **retinal vascular occlusions** by identifying leaks, non-perfusion areas, and abnormal vessel growth. *Ciliary vasculature* - The **ciliary body vasculature** is not directly visualized by standard fluorescein angiography as it is located anterior to the retina within the uveal tract. - While some dye may perfuse the ciliary body, the primary imaging target and diagnostic utility of fluorescein angiography are the **retinal and choroidal circulations**. *Corneal vasculature* - The normal **cornea is avascular**, meaning it does not contain blood vessels. - **Corneal neovascularization** (new vessel growth) can occur due to pathology, but fluorescein angiography is not the primary or most suitable technique for assessing corneal vessels, which are more readily visible with slit-lamp biomicroscopy. *Conjunctival vasculature* - The **conjunctiva** contains numerous small vessels, but these are superficial and can be directly observed with a slit lamp or even the naked eye. - Fluorescein angiography is an invasive procedure with a higher spatial resolution designed for deeper, more intricate vascular networks like those in the retina, making it overkill and inappropriate for routine assessment of the **conjunctival vasculature**.
Radiology
4 questionsBarium swallow is used for -
"String of beads" appearance on horizontal abdominal view X-ray is suggestive of:
What condition is indicated by the double bubble sign on an abdominal X-ray?
Investigation with least radiation dose in the diagnosis of Meckel's diverticulum is -
NEET-PG 2013 - Radiology NEET-PG Practice Questions and MCQs
Question 1281: Barium swallow is used for -
- A. Colon
- B. Esophagus (Correct Answer)
- C. Duodenum
- D. Jejunum
Explanation: ***Esophagus*** - A **barium swallow** specifically visualizes the **esophagus**, pharynx, and sometimes the early stomach. - It's used to identify abnormalities like **dysphagia**, strictures, **achalasia**, or tumors by coating the mucosal lining. *Colon* - The colon is typically examined using a **barium enema**, where barium sulfate is administered rectally. - This procedure is effective for visualizing the large intestine for conditions like **polyps**, diverticula, or inflammatory bowel disease. *Duodenum* - While a barium swallow may transiently show the **duodenum**, its primary target is the esophagus and stomach. - More detailed imaging of the duodenum often requires an **upper GI series (UGI)**, which is a broader study of the upper digestive tract. *Jejunum* - The jejunum is part of the small intestine and is best visualized through a **small bowel follow-through (SBFT)** procedure. - This involves ingesting barium and taking serial X-rays as it progresses through the small bowel, to detect conditions like **Crohn's disease** or obstructions.
Question 1282: "String of beads" appearance on horizontal abdominal view X-ray is suggestive of:
- A. Intussusception
- B. Sigmoid volvulus
- C. Small bowel obstruction (Correct Answer)
- D. Large bowel obstruction
Explanation: ***Small bowel obstruction*** - A "string of beads" appearance on a horizontal abdominal view X-ray refers to small gas bubbles trapped between the valvulae conniventes in a dilated small bowel loop. - This finding is highly suggestive of **complete small bowel obstruction**, particularly when accompanied by multiple air-fluid levels and dilated bowel loops. *Intussusception* - While it causes obstruction, intussusception usually appears as a **target sign** (doughnut sign) on ultrasound or a **meniscus sign** on barium enema, not a string of beads on plain X-ray. - Plain X-rays may show signs of **bowel obstruction**, but the string of beads is not characteristic. *Sigmoid volvulus* - Sigmoid volvulus is characterized by a **dilated loop of colon** forming an inverted U-shape, often described as a **coffee bean sign** or **omega sign**, on plain X-ray. - This involves the large bowel, and the "string of beads" specifically relates to gas in the small bowel. *Large bowel obstruction* - Large bowel obstruction typically presents with a **dilated colon** proximal to the obstruction and a collapsed distal colon, often with absent or minimal gas in the rectum and sigmoid. - While air-fluid levels can be present, the "string of beads" is a specific sign of gas within dilated small bowel loops, distinguishing it from most large bowel obstructions.
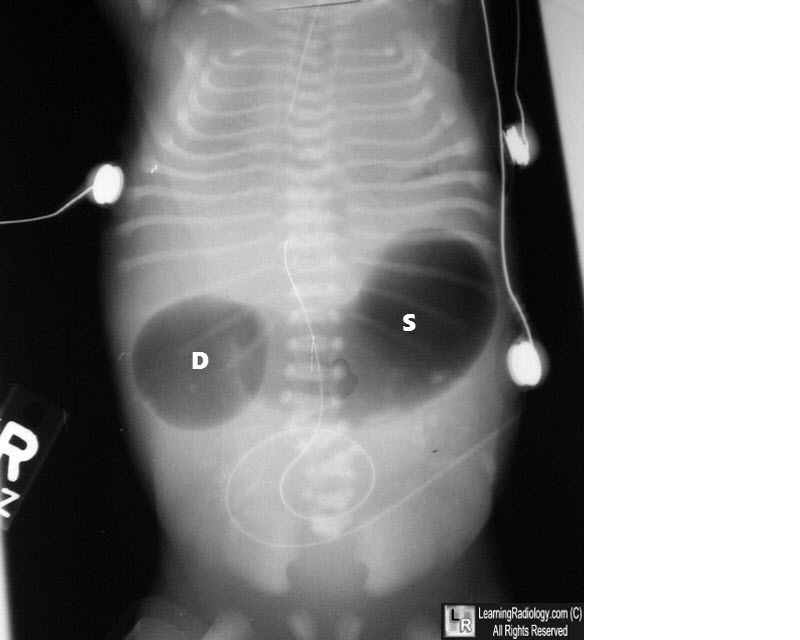
Question 1283: What condition is indicated by the double bubble sign on an abdominal X-ray?
- A. Duodenal stenosis
- B. Volvulus
- C. All of the options
- D. Duodenal atresia (Correct Answer)
Explanation: ***Duodenal atresia*** - The **double bubble sign** on an abdominal X-ray is pathognomonic for **duodenal atresia**, characterized by two air-filled bubbles: one in the stomach and one in the proximal duodenum, separated by the pylorus. - This congenital anomaly results from a complete obstruction of the duodenum, preventing the passage of air and fluid past this point. *Duodenal stenosis* - While also an obstruction of the duodenum, **duodenal stenosis** is an incomplete obstruction, meaning some gas will pass beyond the duodenum. - This would result in gas being present in the distal bowel, which is not seen with a classic "double bubble" where the bowel distal to the duodenum is gasless. *Volvulus* - **Volvulus** involves the twisting of a loop of intestine, leading to obstruction and potentially ischemia. - While it can cause obstruction, it typically presents with a "corkscrew" appearance on an upper GI series or signs of diffuse bowel distension, not the isolated double bubble. *All of the options* - The double bubble sign is highly specific to **duodenal atresia** due to the complete obstruction it signifies. - Other conditions like duodenal stenosis and volvulus cause different radiological patterns, making this option incorrect.
Question 1284: Investigation with least radiation dose in the diagnosis of Meckel's diverticulum is -
- A. MRI
- B. CT
- C. Contrast radiography
- D. Technetium -99m scanning (Correct Answer)
Explanation: ***Technetium-99m scanning*** - **Technetium-99m pertechnetate scan** (Meckel's scan) is the **gold standard investigation** for diagnosing Meckel's diverticulum with ectopic gastric mucosa - Among the investigations that can actually **diagnose Meckel's diverticulum**, it has the **lowest radiation dose** (approximately 1-2 mSv) - The radioisotope is specifically taken up by ectopic gastric mucosa, providing both diagnostic utility and relatively low radiation exposure - **Sensitivity: 85-95%** for detecting ectopic gastric mucosa in Meckel's diverticulum - The radiation dose is comparable to a few months of natural background radiation and significantly lower than CT or contrast studies *MRI* - While **MRI uses no ionizing radiation**, it is **not a standard or practical investigation** for diagnosing Meckel's diverticulum - MRI cannot identify ectopic gastric mucosa specifically - It is rarely used in clinical practice for this indication - The question asks about investigation "in the diagnosis" of Meckel's diverticulum, implying a test that is actually used diagnostically *CT* - **Computed Tomography (CT)** delivers a **high radiation dose** (typically 5-10 mSv or more) - While it can identify structural abnormalities, it is not specific for Meckel's diverticulum - Not the first-line investigation for this condition *Contrast radiography* - **Contrast studies** (barium studies) use **moderate ionizing radiation** (3-5 mSv) - Limited utility in diagnosing Meckel's diverticulum as it primarily assesses luminal patency - Cannot identify ectopic gastric mucosa - Lower sensitivity compared to Tc-99m scanning
Surgery
1 questionsPulled up cecum is seen in which condition?
NEET-PG 2013 - Surgery NEET-PG Practice Questions and MCQs
Question 1281: Pulled up cecum is seen in which condition?
- A. Cecal carcinoma
- B. Intussusception
- C. Colon carcinoma
- D. Ileocecal tuberculosis (TB) (Correct Answer)
Explanation: ***Ileocecal tuberculosis (TB)*** - **Ileocecal tuberculosis** commonly causes **fibrosis** and stricture formation in the ileocecal region, which can lead to the **retraction or pulling up of the cecum**. - This "pulled-up cecum" is a characteristic radiographic finding, often associated with a **patulous ileocecal valve** and inflammatory changes. *Cecal carcinoma* - While cecal carcinoma can cause a mass and involve the cecum, it does not typically lead to a "pulled-up" appearance. - Carcinoma usually presents as a **filling defect** or an **obstructing lesion** rather than retraction. *Intussusception* - **Intussusception** involves the telescoping of one part of the intestine into another, usually presenting as a **target sign** on imaging. - This condition does not cause a *pulled-up cecum*; instead, it involves the distal segment invaginating into the proximal segment. *Colon carcinoma* - **Colon carcinoma** can manifest as an **apple-core lesion** or an obstructing mass, but like cecal carcinoma, it generally does not cause the cecum to be pulled upwards. - The pathology is primarily one of **luminal narrowing** or mass obstruction.