What is the recommended time frame for completing a blood transfusion after initiation?
What is the recommended rate of correction for sodium deficit in patients with chronic hyponatremia?
Graham Steell murmur is associated with which of the following conditions?
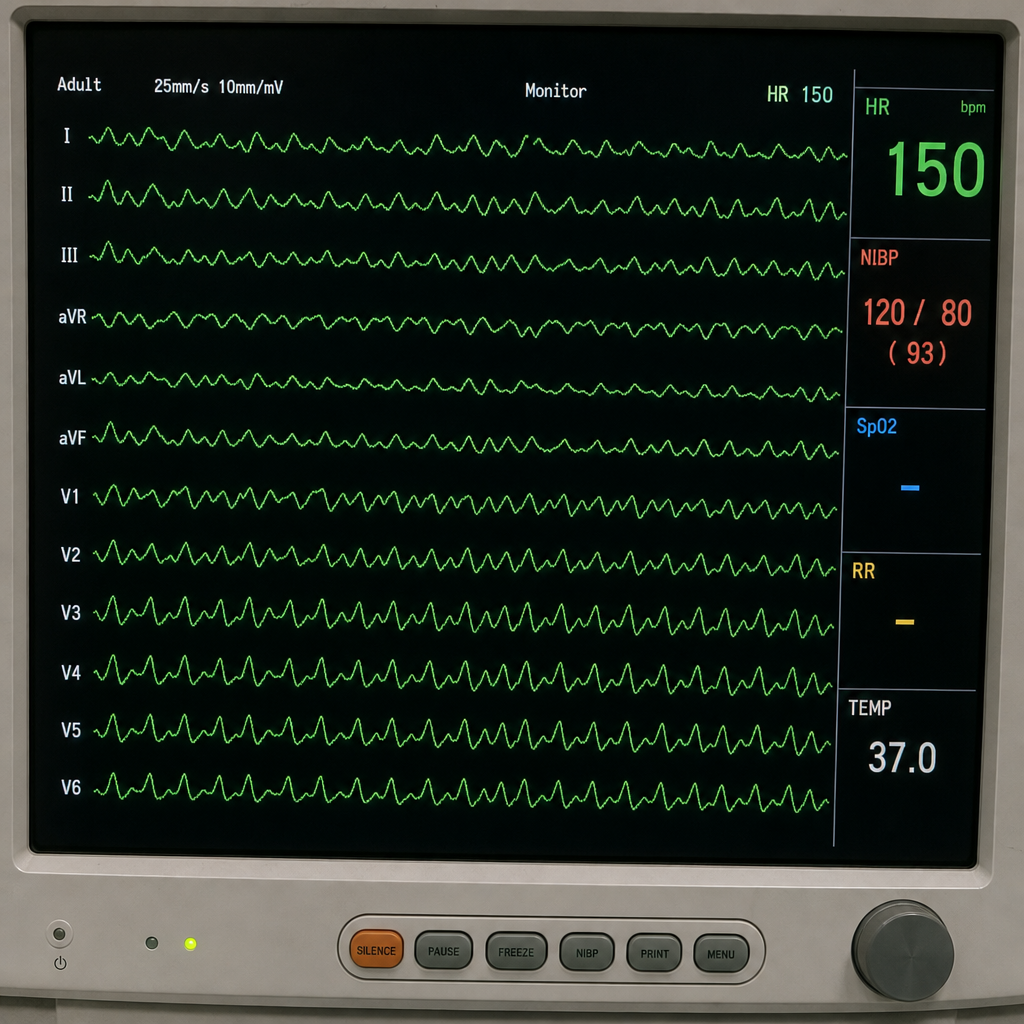
Refer to the provided ECG image. It demonstrates which of the following?
Wireless capsule endoscopy is done to visualize which of the following condition?
In a patient with heart disease, which condition is most commonly associated with left atrial enlargement?
Lovibond profile sign is seen in ?
All are seen in Behçet's syndrome except:
Match stick test is positive in ?
Which of the following is a characteristic feature of Granulomatosis with polyangiitis?