Clinical Manifestations and Presentation of Diseases — MCQs

On this page
Heerfordt's syndrome consists of fever, parotid enlargement, facial palsy, and which of the following?
25-year-old male having fever and malaise for 2 weeks, arthritis of the ankle joint, and tender erythematous nodules over the shin. What is the diagnosis?
Most common cause of postural hypotension is
Kartagener's syndrome includes all of the following conditions except.
Which of the following is NOT typically associated with carcinoma of the pancreas?
A 20-year-old girl presents with abdominal pain and a purpuric rash all over the body, and the most probable diagnosis is?
Which of the following conditions can be associated with the presence of erythema nodosum?
A patient complains of loss of visual acuity, deafness, and enlargement of the maxilla.
Which of the following conditions is associated with acanthosis nigricans?
Which condition is primarily associated with Letessier-Meige disease?
Clinical Manifestations and Presentation of Diseases Indian Medical PG Practice Questions and MCQs
Question 311: Heerfordt's syndrome consists of fever, parotid enlargement, facial palsy, and which of the following?
- A. Facial palsy
- B. Uveitis (Correct Answer)
- C. Fever
- D. Parotid enlargement
Explanation: ***Uveitis*** - **Heerfordt's syndrome** is a rare manifestation of **sarcoidosis**, classically characterized by a tetrad of symptoms: **fever**, **parotid gland enlargement**, **facial nerve palsy**, and **uveitis**. - **Uveitis** (inflammation of the uvea of the eye) is a key component differentiating this syndrome. *Fever* - **Fever** is one of the four defining components of Heerfordt's syndrome, but it is not the *missing* component being asked for in the question. - The question asks for the additional symptom that, along with the others listed, completes the syndrome. *Parotid enlargement* - **Parotid enlargement** (inflammation and swelling of the parotid glands) is another established component of Heerfordt's syndrome. - It's already mentioned in the question stem as one of the symptoms present. *Facial palsy* - **Facial palsy** (weakness or paralysis of the facial muscles, often unilateral) is also a classic feature of Heerfordt's syndrome. - This symptom is explicitly mentioned in the question as one of the presenting features.
Question 312: 25-year-old male having fever and malaise for 2 weeks, arthritis of the ankle joint, and tender erythematous nodules over the shin. What is the diagnosis?
- A. Erythema nodosum (Correct Answer)
- B. Weber- Christian disease
- C. Nodular Vasculitis
- D. Hansen's disease
Explanation: ***Erythema nodosum*** - Erythema nodosum presents with **tender, erythematous nodules** on the shins, often associated with a **prodrome of fever and malaise**, and can be accompanied by **arthralgia or arthritis**, particularly in the ankle joint [1]. - It is a **panniculitis** (inflammation of subcutaneous fat) that can be triggered by various systemic conditions, infections, or drugs. *Hansen's disease* - Also known as **leprosy**, this infectious disease primarily affects the skin, peripheral nerves, upper respiratory tract, eyes, and testes, typically presenting with **hypopigmented skin lesions** with loss of sensation. - While it can cause skin nodules (lepromas) and nerve damage leading to joint deformities, the acute onset of tender erythematous shin nodules accompanying a generalized inflammatory response is **not characteristic** of its initial presentation. *Weber-Christian disease* - This is a rare, relapsing, febrile **panniculitis** that causes subcutaneous fat inflammation, often resulting in tender nodules or plaques, but it is not typically associated with prominent arthralgia/arthritis as primary symptoms. - The lesions tend to be more widespread than just the shins and can involve visceral fat, and it lacks the specific association with ankle arthritis seen in erythema nodosum. *Nodular Vasculitis* - This condition is a form of **cutaneous vasculitis** that presents with multiple, tender, often ulcerating nodules, typically on the lower legs, which are characterized by inflammation of blood vessels. - While it involves nodules, it is fundamentally a vasculitic process and usually presents with symptoms of **vascular damage** such as ulcers, purpura, or livedo reticularis, which are not described in the patient's presentation of fever, malaise, and arthritis.
Question 313: Most common cause of postural hypotension is
- A. Progressive cerebellar degeneration
- B. Adrenal insufficiency
- C. Striatonigral degeneration
- D. Peripheral neuropathy (Correct Answer)
Explanation: ***Peripheral neuropathy*** - Damage to **autonomic nerve fibers** in peripheral neuropathy can impair the body's ability to regulate **blood pressure** in response to gravitational changes upon standing [1]. - This leads to a failure of **vasoconstriction** and an inadequate increase in **heart rate**, resulting in a significant drop in blood pressure. *Progressive cerebellar degeneration* - This condition primarily affects **coordination** and **balance**, often leading to **ataxia** and dysarthria. - While it can manifest with various neurological symptoms, **postural hypotension** is not its most common or direct consequence. *Adrenal insufficiency* - **Adrenal insufficiency** results in inadequate production of **cortisol** and **aldosterone**, leading to **hypotension** and **volume depletion**. - While it causes hypotension, it is not the most frequent cause of **postural hypotension** across the general population. *Striatonigral degeneration* - Also known as **multiple system atrophy** (MSA-P), this condition involves the degeneration of neurons in the **striatum** and **substantia nigra**. - It often leads to **parkinsonism** and **autonomic dysfunction**, including postural hypotension, but it is less common overall than peripheral neuropathy as a cause.
Question 314: Kartagener's syndrome includes all of the following conditions except.
- A. Situs inversus
- B. Bronchiectasis
- C. Sinusitis
- D. Cystic fibrosis (Correct Answer)
Explanation: ***Cystic fibrosis*** - Cystic fibrosis is a genetic disorder affecting mucus and sweat glands, characterized by excessive secretions that lead to blockages in various organs, including the lungs and pancreas. This is a distinct condition from Kartagener's syndrome. - While both conditions can present with chronic respiratory infections, **cystic fibrosis** is caused by mutations in the **CFTR gene**, and is not a component of Kartagener's syndrome or primary ciliary dyskinesia [1]. *Situs inversus* - **Situs inversus** is a characteristic feature of Kartagener's syndrome, occurring in about 50% of affected individuals due to immotile cilia during embryonic development, leading to reversed organ placement. - The abnormal ciliary function prevents the proper rotation of organs during embryogenesis, resulting in **dextrocardia** and the transposition of abdominal organs. *Bronchiectasis* - **Bronchiectasis** is a common complication of Kartagener's syndrome, resulting from chronic inflammation and infection in the airways due to impaired mucociliary clearance. - The inability of cilia to effectively clear mucus and pathogens leads to recurrent infections, chronic inflammation, and irreversible dilation of the bronchi, a hallmark of **bronchiectasis** [1]. *Sinusitis* - **Sinusitis** is frequently observed in patients with Kartagener's syndrome because the dysfunctional cilia in the paranasal sinuses fail to clear mucus and trapped pathogens, leading to chronic inflammation and infection. - This chronic inflammation often presents as **recurrent or persistent sinus infections** and can be severe and difficult to treat due to the underlying ciliary defect.
Question 315: Which of the following is NOT typically associated with carcinoma of the pancreas?
- A. Hypercalcemia
- B. Erythrocytosis
- C. Syndrome of inappropriate secretion of ADH
- D. Hypoglycemia (Correct Answer)
Explanation: ***Hypoglycemia*** - **Hypoglycemia** is generally not a direct paraneoplastic syndrome or common complication of typical pancreatic adenocarcinoma. - While **insulinomas** (a rare type of pancreatic neuroendocrine tumor) cause hypoglycemia, they are distinct from pancreatic adenocarcinoma [1]. *Syndrome of inappropriate secretion of ADH* - **SIADH** can be a paraneoplastic syndrome, causing **hyponatremia** due to excessive ADH secretion. - Although less common than in small cell lung cancer, some pancreatic cancers can produce **ectopic ADH**. *Erythrocytosis* - Some tumors, including certain pancreatic cancers, can produce **erythropoietin** leading to **erythrocytosis** (an increase in red blood cell mass). - This is a paraneoplastic syndrome reflecting excessive red blood cell production. *Hypercalcemia* - **Hypercalcemia of malignancy** is a well-recognized paraneoplastic syndrome that can occur with various cancers, including pancreatic cancer. - It can result from **parathyroid hormone-related peptide (PTHrP) production** by the tumor or extensive bony metastases.
Question 316: A 20-year-old girl presents with abdominal pain and a purpuric rash all over the body, and the most probable diagnosis is?
- A. Hemolytic Uremic Syndrome (HUS)
- B. Kawasaki Syndrome
- C. Immune Thrombocytopenic Purpura (ITP)
- D. Henoch-Schönlein Purpura (HSP) (Correct Answer)
Explanation: ***Henoch-Schönlein Purpura (HSP)*** - The classic triad of **abdominal pain**, **arthralgia** (often knee and ankle), and a **palpable purpuric rash**, particularly on the lower extremities and buttocks, strongly points to HSP [2]. - This is a **small vessel vasculitis** mediated by IgA immune complex deposition [1], [2]. *Hemolytic Uremic Syndrome (HUS)* - HUS is characterized by a triad of **microangiopathic hemolytic anemia**, **thrombocytopenia**, and **acute kidney injury**, often preceded by bloody diarrhea due to Shiga-toxin producing *E. coli* [3]. - While it can cause abdominal pain and purpura-like lesions (due to thrombocytopenia), the specific presentation here is more indicative of HSP. *Kawasaki Syndrome* - Kawasaki disease is a **medium-vessel vasculitis** primarily affecting young children, characterized by fever, conjunctivitis, oral mucosal changes, rash, lymphadenopathy, and extremity changes [4]. - It does not typically present with the same type of palpable purpuric rash or severe abdominal pain described in this case. *Immune Thrombocytopenic Purpura (ITP)* - ITP is an **isolated thrombocytopenia** (low platelet count) leading to increased bleeding tendency, presenting as petechiae, purpura, and mucosal bleeding. - While purpura is present, the additional finding of significant **abdominal pain** points away from isolated ITP and towards a systemic vasculitis like HSP.
Question 317: Which of the following conditions can be associated with the presence of erythema nodosum?
- A. Tuberculosis
- B. Sarcoidosis
- C. Malignancies
- D. All of the options (Correct Answer)
Explanation: ***All of the options*** - **Erythema nodosum** is a common panniculitis that can be associated with a wide range of underlying conditions, including infections, inflammatory diseases, and malignancies. - Therefore, **tuberculosis**, **sarcoidosis**, and various types of **malignancies** are all known causes or associations of erythema nodosum [1]. *Tuberculosis* - **Tuberculosis (TB)**, particularly primary infection or reactivation, is a well-established infectious cause of **erythema nodosum**, especially in endemic areas. - The immune response to the **mycobacterial antigens** can trigger the characteristic tender, red nodules, often on the shins. *Sarcoidosis* - **Sarcoidosis** is a systemic granulomatous disease that frequently presents with **erythema nodosum**, particularly in acute forms like **Löfgren's syndrome** [1]. - In such cases, erythema nodosum is often accompanied by **hilar adenopathy** and **arthralgia**. *Malignancies* - Various **malignancies**, including **lymphomas**, **leukemias**, and even some solid tumors, can rarely be associated with **erythema nodosum** as a paraneoplastic phenomenon [1]. - The development of erythema nodosum in these contexts is thought to be due to immune reactions to **tumor antigens** or direct involvement of skin by the malignancy.
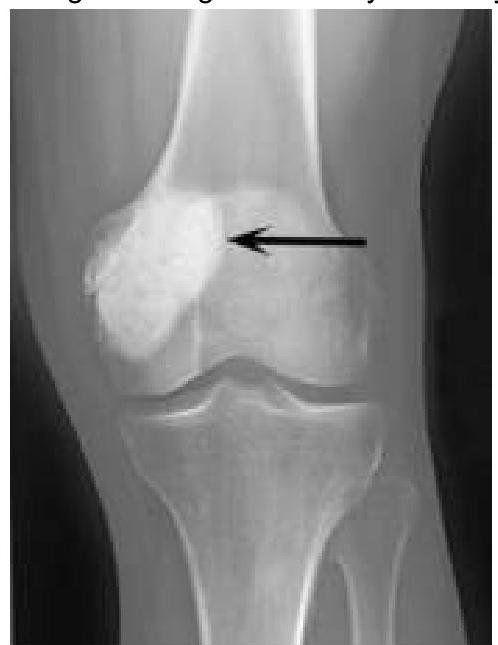
Question 318: A patient complains of loss of visual acuity, deafness, and enlargement of the maxilla.
- A. Fibrous dysplasia
- B. Osteogenesis imperfecta
- C. Paget's disease (Correct Answer)
- D. Osteomalacia
Explanation: ***Paget's disease*** [1] - Characterized by abnormal **bone remodeling**, leading to an increase in bone size and deformity, particularly in the **maxilla**, causing enlargement [1]. - Associated with complications such as **loss of visual acuity** (due to involvement of the skull) and **deafness** from auditory canal changes [1][2], making this the most fitting diagnosis. *Fibrous dysplasia* - Typically presents with **fibrous replacement** of bone, not specifically causing deafness or visual acuity loss. - Customarily involves the **classic "ground glass" appearance** on imaging, not the structural enlargement seen in Paget's disease. *Osteogenesis imperfecta* - Mainly causes **brittle bones** and frequent fractures, not associated with **maxillary enlargement** or changes in auditory function. - Rarely causes visual acuity loss, which is not a feature of this condition. *Osteomalacia* - Primarily characterized by **softening of bones** due to vitamin D deficiency, leading to weakness rather than structural changes like maxillary enlargement. - Symptoms like **bone pain** or **muscle weakness** occur, but not specifically loss of auditory function or visual acuity. **References:** [1] Kumar V, Abbas AK, et al.. Robbins and Cotran Pathologic Basis of Disease. 9th ed. Bones, Joints, and Soft Tissue Tumors, pp. 1192-1194. [2] Cross SS. Underwood's Pathology: A Clinical Approach. 6th ed. Common Clinical Problems From Osteoarticular And Connective Tissue Disease, pp. 669-670.
Question 319: Which of the following conditions is associated with acanthosis nigricans?
- A. Obesity
- B. Gastric adenocarcinoma
- C. Type 2 Diabetes Mellitus (Correct Answer)
- D. All of the options
Explanation: Acanthosis nigricans is characterized by velvety, hyperpigmented skin lesions, often in intertriginous areas, and is a common cutaneous marker for insulin resistance, which is central to Type 2 Diabetes Mellitus [1]. The elevated insulin levels stimulate epidermal keratinocytes and dermal fibroblast proliferation, leading to the characteristic skin changes. While malignant acanthosis nigricans is associated with internal malignancies, particularly adenocarcinomas of the gastrointestinal tract (like gastric), it is a less common cause than insulin resistance. This form is usually more extensive and rapidly progressing than the benign variant. Obesity is strongly associated with insulin resistance, making it an indirect cause of acanthosis nigricans. However, acanthosis nigricans is a direct indicator of insulin resistance, which can occur with or without significant obesity. While all listed conditions can be associated with acanthosis nigricans, Type 2 Diabetes Mellitus is the most direct and common condition explicitly linked to the underlying pathophysiology of insulin resistance [1]. Gastric adenocarcinoma causes a malignant form, and obesity is a risk factor for insulin resistance, but T2DM directly reflects the metabolic state responsible for the skin changes.
Question 320: Which condition is primarily associated with Letessier-Meige disease?
- A. Lymphedema (Correct Answer)
- B. A-V malformations
- C. Chronic venous insufficiency
- D. Abdominal aortic aneurysm
Explanation: ***Lymphedema*** - **Letessier-Meige disease**, also known as **primary lymphedema type I** or **Meige disease**, is a congenital form of lymphedema. - It is caused by **hypoplasia** or malformation of the lymphatic vessels, leading to chronic swelling, typically in the lower limbs. *A-V malformations* - **Arteriovenous malformations** are abnormal connections between arteries and veins, bypassing the capillary system. - They are distinct from lymphatic system disorders and can cause symptoms related to shunting blood, such as bleeding or heart failure. *Abdominal aortic aneurysm* - An **abdominal aortic aneurysm** is a localized dilation of the abdominal aorta due to weakening of the vessel wall. - This condition is a vascular disease involving arteries, with no direct association with lymphatic system dysfunction. *Chronic venous insufficiency* - **Chronic venous insufficiency** results from incompetent venous valves, leading to blood pooling in the veins, particularly in the lower extremities. - While it can cause leg swelling, it is a disorder of the venous system rather than the lymphatic system, which is affected in Letessier-Meige disease.
Practice by Chapter
Approach to Common Symptoms (Fever, Pain, Fatigue)
Practice Questions
Constitutional Symptoms and Their Differential Diagnosis
Practice Questions
Syncope and Presyncope
Practice Questions
Dizziness and Vertigo
Practice Questions
Dyspnea and Respiratory Distress
Practice Questions
Chest Pain Evaluation
Practice Questions
Abdominal Pain Assessment
Practice Questions
Headache Classification and Management
Practice Questions
Weight Loss and Cachexia
Practice Questions
Edema and Fluid Retention
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Start For Free