Tetanic contraction is due to accumulation of?
What percentage of gastric secretion is attributed to the cephalic phase?
Which hormone primarily inhibits gastric acid secretion in response to acidic chyme?
Prostaglandins (PGs) in semen are secreted by?
Wolff–Chaikoff effect is due to?
Growth hormone level is highest during
Insensible water loss per day is ?
Which of the following factors increases the rate of particle diffusion across the cell membrane?
Gas exchange in tissues takes place at?
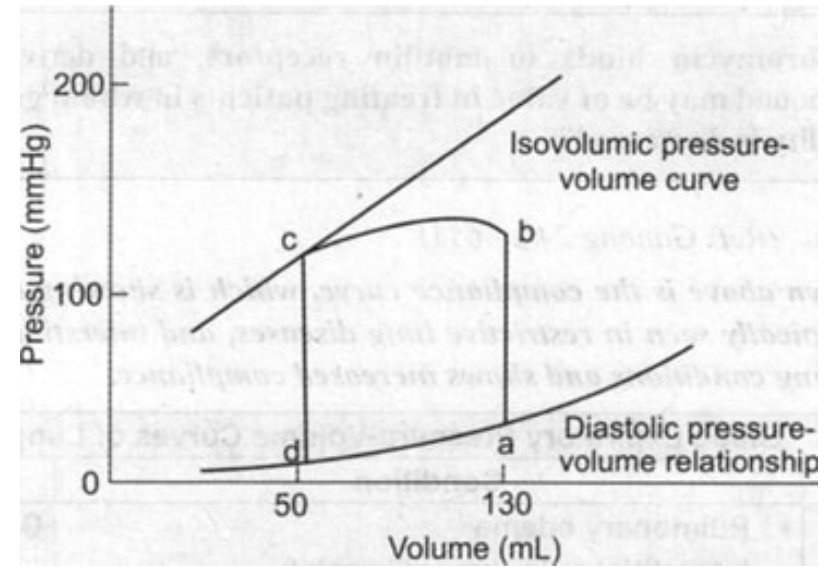
From the given pressure-volume curve, identify the end-diastolic volume (EDV) and end-systolic volume (ESV), then calculate the ejection fraction using the formula EF = (EDV - ESV)/EDV × 100%.