Pediatric HIV Indian Medical PG Practice Questions and MCQs
Practice Indian Medical PG questions for Pediatric HIV. These multiple choice questions (MCQs) cover important concepts and help you prepare for your exams.
Pediatric HIV Indian Medical PG Question 1: In an infant born to a HIV infected mother, at what age can the ELISA test reliably diagnose HIV infection?
- A. 18 months (Correct Answer)
- B. 3 months
- C. 9 months
- D. 12 months
Pediatric HIV Explanation: ***18 months***
- At **18 months of age**, maternal HIV antibodies passed to the infant are usually no longer present, allowing for accurate detection of the infant's own antibody response via ELISA.
- Before this age, a positive ELISA test might reflect the presence of **maternal antibodies** rather than true infant infection.
*3 months*
- An ELISA test at 3 months would not reliably diagnose HIV infection as **maternal antibodies** are still typically present in the infant's system.
- Early diagnosis in infants usually requires **virological tests** (e.g., PCR for HIV DNA or RNA) that detect the virus itself, not antibodies.
*9 months*
- While maternal antibodies may start to wane by 9 months, they can still be present, leading to **false positive** ELISA results.
- Virological testing remains the preferred method for definitive diagnosis before 18 months.
*12 months*
- A significant proportion of infants may still have detectable **maternal antibodies** at 12 months, making ELISA unreliable for true infection diagnosis.
- Confirmation of HIV infection at this age would still ideally involve **virological testing**.
Pediatric HIV Indian Medical PG Question 2: What is the recommended regimen for post-exposure prophylaxis for HIV?
- A. Zidovudine + Lamivudine + Lopinavir/ritonavir for 28 days
- B. Tenofovir disoproxil fumarate + Emtricitabine + Raltegravir for 28 days
- C. Single dose Tenofovir + Emtricitabine + Raltegravir
- D. Tenofovir disoproxil fumarate + Emtricitabine + Dolutegravir for 28 days (Correct Answer)
Pediatric HIV Explanation: ***Tenofovir disoproxil fumarate + Emtricitabine + Dolutegravir for 28 days***
- This is the **current first-line recommended regimen** for **HIV post-exposure prophylaxis (PEP)** according to WHO (2021), CDC, and Indian NACO guidelines.
- It includes two **nucleoside reverse transcriptase inhibitors (NRTIs)** and an **integrase strand transfer inhibitor (INSTI)**.
- **Dolutegravir** is preferred over Raltegravir due to **superior efficacy, better tolerability, higher barrier to resistance, once-daily dosing**, and fewer drug interactions.
- The duration of **28 days** is crucial for effective PEP to cover the window period for potential HIV integration and replication.
*Tenofovir disoproxil fumarate + Emtricitabine + Raltegravir for 28 days*
- This was the **previous standard PEP regimen** and is still an acceptable alternative if Dolutegravir is contraindicated or unavailable.
- Raltegravir requires **twice-daily dosing** compared to Dolutegravir's once-daily regimen, which may affect adherence.
- The 28-day duration is correct, but Raltegravir is no longer the first-line INSTI choice in current guidelines.
*Single dose Tenofovir + Emtricitabine + Raltegravir*
- A **single dose** of these medications is insufficient for **post-exposure prophylaxis (PEP)** as HIV replication needs to be suppressed over an extended period to prevent seroconversion.
- PEP typically requires a **28-day course** to be effective.
*Zidovudine + Lamivudine + Lopinavir/ritonavir for 28 days*
- While this is an older, effective **antiretroviral regimen**, it is **not the preferred first-line PEP regimen** due to a higher incidence of side effects, particularly with zidovudine (anemia, nausea).
- Modern guidelines favor regimens with **Tenofovir/Emtricitabine + Dolutegravir** due to better tolerability and superior efficacy.
Pediatric HIV Indian Medical PG Question 3: Which of the following methods is NOT recommended for the diagnosis of HIV infection in a 2-month-old child?
- A. Viral culture
- B. DNA-PCR
- C. P24 antigen assay
- D. HIV ELISA (Correct Answer)
Pediatric HIV Explanation: ***HIV ELISA***
- **HIV ELISA** (Enzyme-linked Immunosorbent Assay) detects **HIV antibodies**, which are maternally derived and can persist in newborns for up to 18 months, leading to **false positive** results.
- Therefore, antibody-based tests are **not suitable** for diagnosing HIV infection in infants under 18 months of age.
*Viral culture*
- **HIV viral culture** can directly detect the presence of replication-competent virus in an infant's blood.
- While sensitive, it is **expensive**, labor-intensive, and takes a long time (several weeks) to obtain results, making it less practical for routine diagnosis.
*DNA-PCR*
- **DNA PCR (Polymerase Chain Reaction)** directly detects **HIV proviral DNA** within infected cells, making it highly specific and sensitive for early infant diagnosis.
- It is currently the **recommended method** for HIV diagnosis in infants and young children, especially in the first few months of life.
*P24 antigen assay*
- The **P24 antigen assay** detects the **core protein of the HIV virus**, indicating active viral replication.
- It can be used for early diagnosis in infants but may be less sensitive than DNA PCR, particularly in the presence of maternal antibodies or during early infection.
Pediatric HIV Indian Medical PG Question 4: Most serious characteristic finding of HIV in children is?
- A. Kaposi sarcoma is common
- B. Cryptococcal diarrhoea is common
- C. Recurrent chest infection (Correct Answer)
- D. Recurrent candidiasis
Pediatric HIV Explanation: ***Recurrent chest infection***
- **Recurrent chest infections**, particularly with common bacterial pathogens, are a hallmark of HIV in children due to their underdeveloped immune systems being further compromised.
- Children with HIV are highly susceptible to respiratory infections such as **pneumonia** and **bronchiolitis**, leading to frequent hospitalizations and poor outcomes.
*Kaposi sarcoma is common*
- **Kaposi sarcoma** is a well-known HIV-associated malignancy, but it is much more prevalent in **HIV-positive adults**, especially men who have sex with men, rather than in children.
- While it can occur in children, it is not considered a *characteristic* or common presenting feature, as other opportunistic infections and non-specific symptoms are far more frequent.
*Cryptococcal diarrhoea is common*
- **Cryptococcal infection** primarily manifests as **meningitis** or disseminated disease, particularly in adults with advanced HIV.
- While gastrointestinal symptoms can occur, **Cryptococcal diarrhea** is not a common or characteristic presentation of HIV in children.
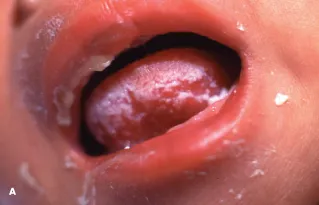
*Recurrent candidiasis*
- While **recurrent oral candidiasis** (thrush) is common in HIV-infected children, it is often one of the **earliest indicators** and can be present even in less advanced disease.
- However, **recurrent chest infections** generally represent a more significant and debilitating manifestation of immune compromise in pediatric HIV.
Pediatric HIV Indian Medical PG Question 5: A term infant is born to a known HIV-positive mother. She has been taking antiretroviral medications for the weeks prior to the delivery of her infant. Routine management of the healthy infant should include which of the following?
- A. HIV ELISA on the infant to determine if congenital infection has occurred
- B. Admission to the neonatal intensive care unit for close cardiovascular monitoring
- C. Chest radiographs to evaluate for congenital Pneumocystis carinii
- D. A course of zidovudine for the infant (Correct Answer)
Pediatric HIV Explanation: ***A course of zidovudine for the infant***
- This is the standard of care for newborns exposed to HIV prenatally, even if the mother received **antiretroviral therapy (ART)**.
- **Zidovudine (AZT)** prophylaxis significantly reduces the risk of **perinatal HIV transmission**.
*HIV ELISA on the infant to determine if congenital infection has occurred*
- **HIV ELISA** tests detect **maternal antibodies** passed to the infant, which can persist for up to 18 months, leading to **false positive results**.
- **HIV DNA PCR** or **RNA assays** are used to diagnose HIV infection in infants.
*Admission to the neonatal intensive care unit for close cardiovascular monitoring*
- Admission to the **NICU** is generally reserved for **premature** or **symptomatic infants**, or those with specific complications.
- A **healthy, term infant** born to an HIV-positive mother on ART does not routinely require NICU admission.
*Chest radiographs to evaluate for congenital Pneumocystis carinii*
- **Pneumocystis jirovecii pneumonia (PJP)** typically presents in HIV-infected infants between **3 to 6 months of age**, not at birth.
- Prophylaxis with **trimethoprim-sulfamethoxazole (TMP-SMX)** is initiated at 4-6 weeks of age for HIV-exposed infants.
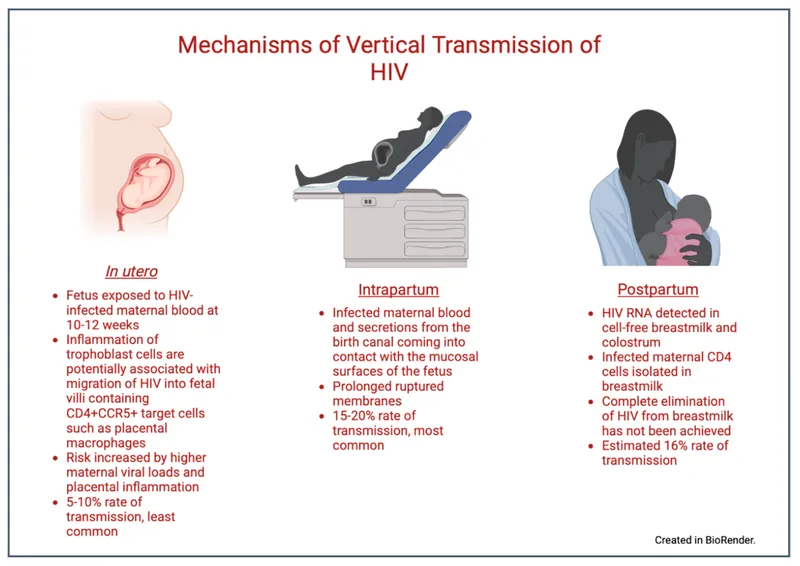
Pediatric HIV Indian Medical PG Question 6: Which of the following is NOT a measure to prevent vertical transmission of HIV?
- A. Stop breast feeding
- B. Vaginal delivery
- C. Administration of vitamin A (Correct Answer)
- D. Treatment with zidovudine
Pediatric HIV Explanation: ***Administration of vitamin A***
- **Vitamin A supplementation** is important for general maternal and child health during pregnancy and lactation.
- However, there is **no evidence** that vitamin A administration has any role in preventing **vertical transmission of HIV**.
- It is **NOT part of PMTCT (Prevention of Mother-to-Child Transmission) protocols**.
*Vaginal delivery*
- **Vaginal delivery increases the risk** of HIV transmission compared to elective cesarean section.
- **Elective cesarean section** (not vaginal delivery) is the preventive measure recommended for mothers with high or unknown viral loads.
- Vaginal delivery may be acceptable only in mothers with **undetectable viral loads** on effective ART.
*Stop breast feeding*
- **Avoiding breastfeeding** (using replacement feeding) is a recognized strategy to prevent **postnatal HIV transmission** in resource-rich settings.
- In resource-limited settings, WHO recommends **exclusive breastfeeding with maternal ART** as the safest option.
- This is part of the comprehensive **PMTCT strategy**.
*Treatment with zidovudine*
- **Zidovudine (AZT)** is a cornerstone of **PMTCT protocols**.
- Administration during pregnancy, labor, and to the newborn **significantly reduces vertical transmission risk**.
- Now often part of combination **antiretroviral therapy (ART)** regimens for pregnant women with HIV.
Pediatric HIV Indian Medical PG Question 7: Prophylaxis with cotrimoxazole is recommended in all situations except for which of the following?
- A. All symptomatic HIV infected children > 5 years of age irrespective of CD4 (Correct Answer)
- B. All HIV infected infants less than 1 year age irrespective of symptoms or CD4 counts
- C. All HIV exposed infants till HIV infection can be ruled out
- D. As secondary prophylaxis after initial treatment for Pneumocystis jirovecii pneumonia
Pediatric HIV Explanation: ***All symptomatic HIV infected children > 5 years of age irrespective of CD4***
- Cotrimoxazole prophylaxis is generally recommended for HIV-infected children with **CD4 counts below certain thresholds** or **specific clinical scenarios**, not just based on age and symptoms alone for those > 5 years.
- The guidelines often focus on preventing **Pneumocystis jirovecii pneumonia (PJP)** and other opportunistic infections in pediatric HIV, with a nuanced approach to older children based on immune status.
*All HIV exposed infants till HIV infection can be ruled out*
- **Cotrimoxazole prophylaxis** is strongly recommended for **all HIV-exposed infants** from 4-6 weeks of age until HIV infection is definitively ruled out.
- This prevents **P. jirovecii pneumonia**, which has a high mortality rate in this vulnerable population.
*All HIV infected infants less than 1 year age irrespective of symptoms or CD4 counts*
- **Cotrimoxazole prophylaxis** is indicated for **all HIV-infected infants younger than 1 year of age**, regardless of their clinical symptoms or CD4 counts.
- This is due to their **immature immune system** and high risk of **opportunistic infections**, especially PJP.
*As secondary prophylaxis after initial treatment for pneumocystis carini pneumonia*
- **Cotrimoxazole** is the **standard drug** used for **secondary prophylaxis** following successful treatment of **Pneumocystis jirovecii pneumonia (PJP)**.
- This prevents recurrence of PJP, which can be life-threatening in immunocompromised individuals.
Pediatric HIV Indian Medical PG Question 8: Best method to diagnose HIV in an infant?
- A. ELISA
- B. PCR (Correct Answer)
- C. Western blot
- D. All of the options
Pediatric HIV Explanation: ***PCR***
- **Polymerase Chain Reaction (PCR)** detects **HIV nucleic acids** (DNA or RNA) directly, which is crucial for infants because maternal antibodies can persist for up to 18 months, interfering with antibody-based tests.
- PCR allows for early diagnosis, often within the first few weeks or months of life, facilitating timely intervention.
*ELISA*
- **Enzyme-linked immunosorbent assay (ELISA)** detects HIV antibodies.
- In infants, ELISA can be misleading due to the presence of **maternal HIV antibodies** transferred across the placenta, making it unreliable for diagnosing active infection.
*Western blot*
- **Western blot** is used to confirm positive ELISA results in adults by detecting specific HIV proteins.
- Like ELISA, it relies on the detection of **antibodies** and is therefore not reliable in infants due to maternally transmitted antibodies.
*All of the options*
- This option is incorrect because **ELISA** and **Western blot** are antibody-based tests that are unreliable in infants due to the presence of **maternal antibodies**.
- Only **PCR** directly detects the virus itself, making it the preferred diagnostic method in this age group.
Pediatric HIV Indian Medical PG Question 9: According to WHO clinical staging of HIV in children oral hairy leukoplakia belongs to which clinical stages?
- A. Clinical stage 1
- B. Clinical stage 3
- C. Clinical stage 4
- D. Clinical stage 2 (Correct Answer)
Pediatric HIV Explanation: ***Clinical stage 2***
- **Oral hairy leukoplakia** is classified under WHO clinical stage 2 for HIV infection, representing mild symptomatic disease with moderate immune compromise.
- Stage 2 includes conditions such as **angular cheilitis**, **papular pruritic eruptions**, **recurrent oral ulcerations**, **herpes zoster**, **lineal gingival erythema**, and **recurrent upper respiratory tract infections**.
- **Note:** Oral hairy leukoplakia is **rare in children** and is more commonly seen in adults with HIV; it is caused by **Epstein-Barr virus** reactivation.
*Clinical stage 1*
- This stage includes **asymptomatic** HIV infection or **persistent generalized lymphadenopathy**.
- Stage 1 represents minimal or no immune compromise with no clinical manifestations requiring intervention.
*Clinical stage 3*
- Clinical stage 3 represents **advanced symptomatic disease** with conditions like **unexplained severe malnutrition**, **unexplained persistent diarrhea**, **oral candidiasis**, **pulmonary tuberculosis**, and **severe recurrent bacterial pneumonia**.
- These conditions indicate more severe immunodeficiency than oral hairy leukoplakia.
*Clinical stage 4*
- Clinical stage 4 represents **severe HIV disease** with AIDS-defining illnesses such as **Pneumocystis jirovecii pneumonia**, **extrapulmonary tuberculosis**, **Kaposi's sarcoma**, **HIV encephalopathy**, **CMV retinitis**, and **disseminated mycobacterial infections**.
- Stage 4 conditions are life-threatening and indicate severe immunosuppression.
Pediatric HIV Indian Medical PG Question 10: Which of the following is NOT a feature of HIV infection in childhood -
- A. Failure to thrive
- B. Hepatomegaly
- C. Kaposi sarcoma (Correct Answer)
- D. Lymphoid interstitial pneumonitis
Pediatric HIV Explanation: ***Kaposi sarcoma***
- While Kaposi's sarcoma is a common HIV-associated malignancy in adults, it is **very rare in HIV-infected children**.
- Its presence in children with HIV usually suggests a **more aggressive and rapidly progressing disease course**, but it is not a typical or common feature.
*Failure to thrive*
- **Failure to thrive** is a very common manifestation of HIV infection in children, often due to **poor nutrient absorption**, increased metabolic demands, and chronic infections.
- It leads to **poor weight gain and growth faltering**, negatively impacting overall development.
*Hepatomegaly*
- **Hepatomegaly**, or an enlarged liver, is a frequent finding in HIV-infected children due to various causes such as **opportunistic infections**, drug side effects, and direct HIV involvement of the liver.
- It can be a clinical sign indicating **inflammation or dysfunction** of the liver.
*Lymphoid interstitial pneumonitis*
- **Lymphoid interstitial pneumonitis (LIP)** is a prevalent pulmonary complication specific to HIV infection in children, characterized by **lymphocytic infiltration of the alveolar septa and peribronchial spaces**.
- It often leads to **chronic cough**, hypoxemia, and is considered an **AIDS-defining condition** in pediatric HIV.
More Pediatric HIV Indian Medical PG questions available in the OnCourse app. Practice MCQs, flashcards, and get detailed explanations.