Bone Mineral Density Assessment Indian Medical PG Practice Questions and MCQs
Practice Indian Medical PG questions for Bone Mineral Density Assessment. These multiple choice questions (MCQs) cover important concepts and help you prepare for your exams.
Bone Mineral Density Assessment Indian Medical PG Question 1: Treatment of post menopausal osteoporosis are all EXCEPT
- A. Estrogen
- B. Magnesium and Zinc (Correct Answer)
- C. Calcium, Vit D supplementation
- D. Raloxifene
Bone Mineral Density Assessment Explanation: ***Magnesium and Zinc***
- While **magnesium** and **zinc** are essential for overall health, their role as primary therapeutic agents for established postmenopausal osteoporosis is **unproven** and is not standard treatment.
- They are considered **trace elements** and their deficiency can affect bone health, but supplementation alone is not sufficient to treat osteoporosis.
*Estrogen*
- **Estrogen replacement therapy** was historically used for postmenopausal osteoporosis due to its role in preventing bone loss, but its use is now limited due to **adverse effects** like increased risk of breast cancer and cardiovascular events [1].
- It is still considered in select cases for symptom relief and bone health, but generally at the lowest effective dose for the shortest duration [1].
*Calcium, Vit D supplementation*
- **Calcium and Vitamin D supplementation** are fundamental components of osteoporosis management by supporting bone mineralization and calcium homeostasis [2].
- Adequate intake is critical for both **prevention** and **treatment**, often used in conjunction with other pharmacologic agents [2].
*Raloxifene*
- **Raloxifene** is a **selective estrogen receptor modulator (SERM)** that acts as an estrogen agonist on bone, thereby reducing bone resorption and increasing bone mineral density [1].
- It is used in the treatment and prevention of postmenopausal osteoporosis, with the added benefit of reducing the risk of invasive breast cancer [1].
Bone Mineral Density Assessment Indian Medical PG Question 2: A 70-year-old female has been on alendronate for 7 years for osteoporosis and now complains of pain in her right thigh. What is the next investigation to be performed?
- A. DEXA scan
- B. Serum vitamin D levels
- C. Serum alkaline phosphate levels
- D. X-ray (Correct Answer)
Bone Mineral Density Assessment Explanation: **X-ray**
- Alendronate, a **bisphosphonate**, is associated with **atypical femoral fractures** after prolonged use, and an X-ray is the most appropriate initial investigation to visualize such a fracture.
- Complaints of thigh pain in a patient on long-term bisphosphonate therapy should prompt imaging to rule out this serious complication.
*DEXA scan*
- A DEXA scan assesses **bone mineral density** but does not provide information about acute fractures or structural integrity in response to specific pain.
- While it's used for osteoporosis diagnosis and monitoring, it won't directly identify an atypical femoral fracture.
*Serum vitamin D levels*
- Maintaining adequate **vitamin D levels** is important for bone health, but its measurement won't explain acute thigh pain or identify a fracture.
- Low vitamin D levels can contribute to osteoporosis but are not the primary cause of pain suggestive of an atypical femoral fracture.
*Serum alkaline phosphate levels*
- **Alkaline phosphatase** levels can be elevated in conditions involving increased bone turnover, such as healing fractures or certain bone diseases.
- However, it is not a direct diagnostic tool for identifying atypical femoral fractures and would not be the first line investigation.
Bone Mineral Density Assessment Indian Medical PG Question 3: A female is on hormone replacement therapy for her menopausal symptoms. She is worried about her bone strength because her mom and sister had osteoporosis after the age of 50. All are given for prevention of osteoporosis along with hormonal replacement therapy, EXCEPT:
- A. Calcium
- B. Vitamin-E (Correct Answer)
- C. Vit.D
- D. None of the options
Bone Mineral Density Assessment Explanation: ***Vitamin-E***
- **Vitamin-E** is an **antioxidant** vitamin that primarily protects cells from oxidative damage.
- It does not play a direct role in **bone metabolism** or the prevention of osteoporosis.
*Calcium*
- **Calcium** is a fundamental component of bone tissue and is essential for maintaining **bone density** [1].
- Adequate calcium intake is crucial for **osteoporosis prevention**, especially in postmenopausal women [1], [2].
*Vit.D*
- **Vitamin D** is essential for **calcium absorption** in the gut and its incorporation into bones.
- Without sufficient Vitamin D, calcium cannot be effectively utilized, leading to compromised **bone health**.
*None of the options*
- This option is incorrect because Vitamin E does not contribute to osteoporosis prevention, making it the correct answer to the "EXCEPT" question.
- Calcium and Vitamin D are both vital for bone strength, so stating that none of the options fit would be inaccurate [1].
Bone Mineral Density Assessment Indian Medical PG Question 4: Which clinical sign is consistently present in all bone fractures?
- A. Tenderness (Correct Answer)
- B. None of the options
- C. Crepitus
- D. Abnormal mobility
Bone Mineral Density Assessment Explanation: ***Tenderness***
- **Tenderness** is the most consistently present sign in all bone fractures due to the rich **periosteal innervation** that responds to trauma and inflammation.
- Even in **hairline fractures**, **stress fractures**, or **impacted fractures** where other signs may be absent, localized tenderness is virtually always present in conscious patients.
*None of the options*
- This option incorrectly suggests no universal sign exists, when **tenderness** is actually the most reliable constant finding.
- While fracture presentations can vary, the **rich nerve supply** of the periosteum ensures tenderness is present even in subtle fractures.
*Crepitus*
- **Crepitus** (grating sensation) occurs only when fractured bone ends rub against each other and requires displacement.
- It is absent in **impacted fractures**, **hairline fractures**, and **greenstick fractures** where bone ends remain aligned or incomplete.
*Abnormal mobility*
- **Abnormal mobility** indicates complete fracture with significant displacement and loss of structural integrity.
- It is absent in **incomplete fractures** (greenstick), **impacted fractures**, and fractures that are well-stabilized by surrounding soft tissues.
Bone Mineral Density Assessment Indian Medical PG Question 5: Drug of choice for post menopausal osteoporosis is
- A. Bisphosphonates (Correct Answer)
- B. Estrogen
- C. Thyroxine
- D. Teriparatide
Bone Mineral Density Assessment Explanation: ***Bisphosphonates***
- **Bisphosphonates** are considered the **first-line therapy** for established postmenopausal osteoporosis due to their proven efficacy in reducing the risk of vertebral and non-vertebral fractures.
- They work by **inhibiting osteoclast activity**, thereby decreasing bone resorption and increasing bone mineral density.
*Estrogen*
- While **estrogen therapy** can prevent osteoporosis, it is generally not the first-line treatment due to potential risks like increased risk of **breast cancer**, **stroke**, and **venous thromboembolism**.
- It is typically reserved for women with severe menopausal symptoms who also require osteoporosis prevention, and often used at the **lowest effective dose for the shortest duration**.
*Thyroxine*
- **Thyroxine** is a hormone used primarily to treat **hypothyroidism**, a condition where the thyroid gland doesn't produce enough thyroid hormone.
- It is **not indicated for the treatment of osteoporosis** and can even worsen bone loss if given in excessive doses, leading to iatrogenic hyperthyroidism.
*Teriparatide*
- **Teriparatide** is an **anabolic agent** that stimulates new bone formation, making it a powerful option for severe osteoporosis or those who have failed other therapies.
- However, it is an injectable medication with a **limited treatment duration** (typically 2 years) and is generally reserved for patients with a **high fracture risk** rather than being the initial drug of choice for all postmenopausal osteoporosis.
Bone Mineral Density Assessment Indian Medical PG Question 6: In Osteoporosis which of these is seen?
- A. Normal calcium, decreased ALP
- B. Decreased calcium, increased ALP
- C. Normal calcium, normal ALP (Correct Answer)
- D. Decreased calcium, decreased ALP
Bone Mineral Density Assessment Explanation: ***Normal calcium, normal ALP***
- In **osteoporosis**, the primary defect is a reduction in **bone mass** due to imbalanced bone remodeling, but the remaining bone tissue is normally mineralized [1].
- Therefore, **serum calcium** and **alkaline phosphatase (ALP)**, which reflect bone turnover and mineralization, typically remain within normal ranges [3].
*Normal calcium, decreased ALP*
- While **serum calcium** is usually normal in osteoporosis, **decreased ALP** is not a characteristic finding.
- Decreased ALP might indicate conditions like **hypophosphatasia** or certain nutritional deficiencies, which are distinct from osteoporosis.
*Decreased calcium, increased ALP*
- **Decreased serum calcium** (hypocalcemia) combined with **increased ALP** is often seen in conditions like **osteomalacia** or **rickets**, where there is defective bone mineralization [2].
- This pattern is not typical of osteoporosis, where the problem is a quantitative reduction in bone, not qualitative mineralization defect [3].
*Decreased calcium, decreased ALP*
- A combination of **decreased calcium** and **decreased ALP** is an unusual biochemical profile in bone disorders.
- It could potentially be seen in severe malnutrition leading to multiple deficiencies, but it is not indicative of osteoporosis.
Bone Mineral Density Assessment Indian Medical PG Question 7: Brittle bone disease is -
- A. Osteoporosis
- B. Pagets disease
- C. Osteopetrosis
- D. Osteogenesis imperfecta (Correct Answer)
Bone Mineral Density Assessment Explanation: ***Osteogenesis imperfecta***
- **Osteogenesis imperfecta** is an inherited disorder characterized by **brittle bones** that fracture easily, due to a defect in **collagen type I** synthesis.
- Patients often present with **blue sclera**, **dentinogenesis imperfecta**, and **hearing loss**, in addition to frequent fractures.
*Osteoporosis*
- **Osteoporosis** is a condition of **decreased bone density**, making bones fragile and prone to fracture, but it is not typically referred to as "brittle bone disease" in the same congenital sense.
- It is more common in older adults and is often related to **hormonal changes** (e.g., post-menopause) or lifestyle factors.
*Paget's disease*
- **Paget's disease of bone** involves abnormal bone remodeling with excessive bone resorption followed by disorganized and expanded bone formation, leading to **enlarged, weakened bones**.
- It typically affects older individuals and can lead to bone pain, deformities, and fractures, but it's not the primary condition associated with "brittle bone disease."
*Osteopetrosis*
- **Osteopetrosis** is characterized by **abnormally dense bones** due to impaired osteoclast function, leading to a buildup of bone.
- While bones are dense, they are also **brittle** and prone to fracture, and the condition is also known as "marble bone disease" rather than "brittle bone disease."
Bone Mineral Density Assessment Indian Medical PG Question 8: Which of the following is an osteoporotic fracture?
- A. Vertebrae (Correct Answer)
- B. Midshaft of Humerus
- C. Glenoid Fracture
- D. Subtrochanteric Fracture
Bone Mineral Density Assessment Explanation: ### **Explanation: Osteoporotic Fractures**
**Osteoporosis** is characterized by reduced bone mineral density (BMD) and micro-architectural deterioration, leading to increased bone fragility. **Fragility fractures** occur due to low-energy trauma (e.g., a fall from standing height) in areas with a high proportion of **trabecular bone**.
#### **1. Why Vertebrae is Correct**
* **Vertebral compression fractures** are the **most common** type of osteoporotic fracture.
* They often occur in the mid-thoracic or thoracolumbar junction (T12-L1).
* Because vertebrae consist largely of trabecular bone, they are highly sensitive to the metabolic changes of osteoporosis. Many are asymptomatic and present as loss of height or **kyphosis (Dowager’s hump)**.
#### **2. Analysis of Incorrect Options**
* **Midshaft of Humerus:** Osteoporotic fractures of the humerus typically occur at the **Proximal Humerus** (surgical neck). Midshaft fractures usually require higher energy trauma or are associated with pathological lesions (like metastases).
* **Glenoid Fracture:** These are rare and usually result from high-energy intra-articular trauma or shoulder dislocations, not metabolic bone thinning.
* **Subtrochanteric Fracture:** While these occur in the femur, they are **atypical** fractures. They are specifically associated with long-term **Bisphosphonate therapy** rather than primary osteoporosis itself. The classic osteoporotic hip fractures are **Neck of Femur** and **Intertrochanteric** fractures.
---
### **High-Yield Clinical Pearls for INI-CET**
* **Common Sites of Osteoporotic Fractures:**
1. **Vertebrae** (Most common overall)
2. **Distal Radius** (Colles’ fracture - earliest to manifest in post-menopausal women)
3. **Neck of Femur** (Highest morbidity/mortality)
4. **Proximal Humerus**
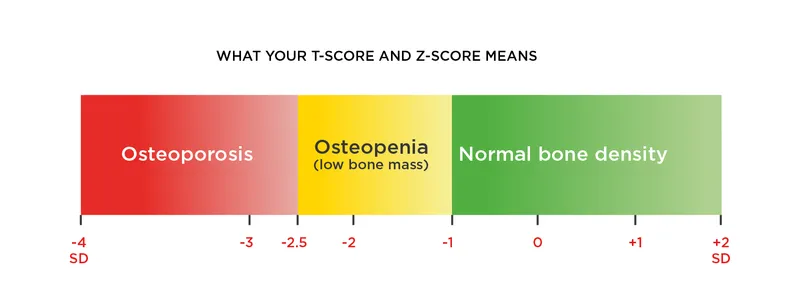
* **Diagnosis:** Gold standard is **DEXA Scan**. Osteoporosis is defined as a **T-score ≤ -2.5**.
* **First-line Treatment:** **Bisphosphonates** (e.g., Alendronate). They inhibit osteoclast-mediated bone resorption.
* **Singh’s Index:** Used to grade osteoporosis based on the disappearance of trabecular patterns in the proximal femur on X-ray.
Bone Mineral Density Assessment Indian Medical PG Question 9: Osteonecrosis is seen in all except
- A. Fracture neck femur
- B. Paget's disease (Correct Answer)
- C. Perthe's disease
- D. Sickle cell anemia
Bone Mineral Density Assessment Explanation: ***Paget's disease***
- **Paget's disease of bone (osteitis deformans)** is a localized disorder of bone remodeling, characterized by excessive and disorganized bone formation, leading to enlarged, softened, and misshapen bones, but not directly causing osteonecrosis.
- While complications like **pathological fractures** and **osteosarcoma** can occur, primary osteonecrosis is not a typical feature of Paget's disease itself.
*Fracture neck femur*
- **Fractures of the femoral neck** can disrupt the blood supply to the femoral head, particularly the medial circumflex femoral artery, leading to **avascular necrosis** (osteonecrosis) of the femoral head.
- This is a well-known and common complication, especially in displaced fractures.
*Sickle cell anemia*
- **Sickle cell anemia** causes sickling of red blood cells, leading to **vaso-occlusion** and impaired blood flow to bones, resulting in **bone infarcts** (osteonecrosis).
- This can affect various bones, including the femoral head, humeral head, and vertebrae.
*Perthe's disease*
- **Perthe's disease** (Legg-Calvé-Perthes disease) is a childhood condition characterized by **idiopathic osteonecrosis** of the femoral head.
- It involves the collapse and subsequent re-ossification of the femoral epiphysis due to an interruption of its blood supply.
Bone Mineral Density Assessment Indian Medical PG Question 10: All of the following statements about HRT (hormone replacement therapy) are true except:
- A. It increases the risk of coronary artery disease
- B. It increases bone mineral density
- C. It increases the risk of breast cancer
- D. It increases the risk of endometrial cancer (Correct Answer)
Bone Mineral Density Assessment Explanation: ***It increases the risk of endometrial cancer***
- This statement is only true for **unopposed estrogen** therapy in women with an intact uterus; combined HRT (estrogen plus progesterone) significantly **reduces** this risk.
- The addition of **progesterone** to estrogen HRT is protective against endometrial hyperplasia and cancer.
*It increases the risk of coronary artery disease*
- Studies have shown that HRT, particularly when initiated several years after menopause, can **increase the risk of cardiovascular events**, including coronary artery disease.
- The **Women's Health Initiative (WHI)** study highlighted these risks, especially in older women starting HRT.
*It increases bone mineral density*
- Estrogen is crucial for maintaining bone density, and HRT can **slow down bone loss** and **reduce the risk of osteoporosis and fractures** in postmenopausal women.
- This is a well-established benefit of HRT for bone health.
*It increases the risk of breast cancer*
- Combined estrogen-progestin HRT has been consistently shown to **increase the risk of breast cancer**, especially with prolonged use (more than 3-5 years).
- This increased risk is a significant concern when considering HRT.
More Bone Mineral Density Assessment Indian Medical PG questions available in the OnCourse app. Practice MCQs, flashcards, and get detailed explanations.