Porphyrias Indian Medical PG Practice Questions and MCQs
Practice Indian Medical PG questions for Porphyrias. These multiple choice questions (MCQs) cover important concepts and help you prepare for your exams.
Porphyrias Indian Medical PG Question 1: A patient's relatives sent a message on social media to the consulting doctor, mentioning that the patient's urinary coproporphyrin test is positive. What is the probable cause?
- A. Lead poisoning (Correct Answer)
- B. Asbestosis
- C. Silicosis
- D. Mercury poisoning
- E. Arsenic poisoning
Porphyrias Explanation: ***Lead poisoning***
- **Lead poisoning** is associated with an increase in **urinary coproporphyrin III**, as lead inhibits the enzyme **coproporphyrinogen oxidase** in the heme synthesis pathway.
- This leads to the accumulation and excretion of **coproporphyrin III** in the urine, making it a valuable biomarker for lead exposure.
*Asbestosis*
- **Asbestosis** is a chronic lung disease caused by inhaling **asbestos fibers**, leading to diffuse interstitial fibrosis.
- It does not directly affect the **heme synthesis pathway** or cause an increase in urinary coproporphyrins.
*Silicosis*
- **Silicosis** is a chronic occupational lung disease caused by inhaling **crystalline silica dust**, resulting in pulmonary fibrosis.
- It is not associated with alterations in **porphyrin metabolism** or increased urinary coproporphyrin levels.
*Mercury poisoning*
- While **mercury poisoning** can affect various organ systems, including renal and neurological, it is not primarily associated with disturbances in the **heme synthesis pathway** or elevated urinary coproporphyrins.
- **Mercury poisoning** often manifests with symptoms like **tremors**, **neurological deficits**, and **kidney damage**.
*Arsenic poisoning*
- **Arsenic poisoning** causes a variety of systemic effects including gastrointestinal symptoms, peripheral neuropathy, and skin changes (hyperpigmentation, hyperkeratosis).
- Unlike lead poisoning, **arsenic does not significantly elevate urinary coproporphyrin III** levels, making it distinguishable from lead toxicity through this biomarker.
Porphyrias Indian Medical PG Question 2: Which is an inhibitor of ferrochelatase ?
- A. Lead (Correct Answer)
- B. Mercury
- C. Iron
- D. Arsenic
Porphyrias Explanation: ***Lead***
- **Lead** is a potent environmental toxin that directly inhibits the enzyme **ferrochelatase**, preventing the insertion of **iron** into **protoporphyrin IX** to form heme.
- This inhibition leads to the accumulation of **protoporphyrin IX** and can cause **anemia** due to impaired **heme synthesis**.
*Mercury*
- While **mercury** is a heavy metal and neurotoxin, its primary mechanism of toxicity does not involve direct inhibition of **ferrochelatase**.
- Its effects are more commonly associated with protein denaturation and enzyme inactivation through binding with **sulfhydryl groups**.
*Iron*
- **Iron** is a substrate for **ferrochelatase**, not an inhibitor. **Ferrochelatase** catalyzes the insertion of **iron** into **protoporphyrin IX** to complete the synthesis of **heme**.
- Deficiencies or excesses of **iron** can affect **heme synthesis**, but **iron** itself does not inhibit the enzyme in a toxic manner.
*Arsenic*
- **Arsenic** is a metalloid that is toxic through various mechanisms, including interference with cellular respiration and DNA repair.
- However, **arsenic** is not known to be a direct inhibitor of **ferrochelatase** in the same way **lead** is.
Porphyrias Indian Medical PG Question 3: Which of the following porphyrias is not inherited as an autosomal dominant disorder?
- A. Porphyria Cutanea Tarda
- B. Hereditary Coproporphyria
- C. Acute Intermittent Porphyria
- D. Congenital Erythropoietic Porphyria (Correct Answer)
Porphyrias Explanation: ***Congenital Erythropoietic Porphyria***
- This porphyria is inherited in an **autosomal recessive** pattern, meaning two copies of the defective gene (one from each parent) are required for the disease to manifest.
- It results from a deficiency in **uroporphyrinogen III synthase (URO-synthase)**, leading to the accumulation of uroporphyrinogen I and coproporphyrinogen I isomers.
*Acute Intermittent Porphyria*
- This is an **autosomal dominant** disorder caused by a deficiency in **hydroxymethylbilane synthase (HMBS)**, also known as porphyrobilinogen deaminase (PBG deaminase).
- It primarily affects the nervous system, leading to acute neurovisceral attacks.
*Porphyria Cutanea Tarda*
- This is **primarily sporadic (acquired)** in about 80% of cases, often associated with hepatic iron overload, alcohol use, hepatitis C, or estrogen use.
- Only about 20% of cases are familial with **autosomal dominant** inheritance pattern.
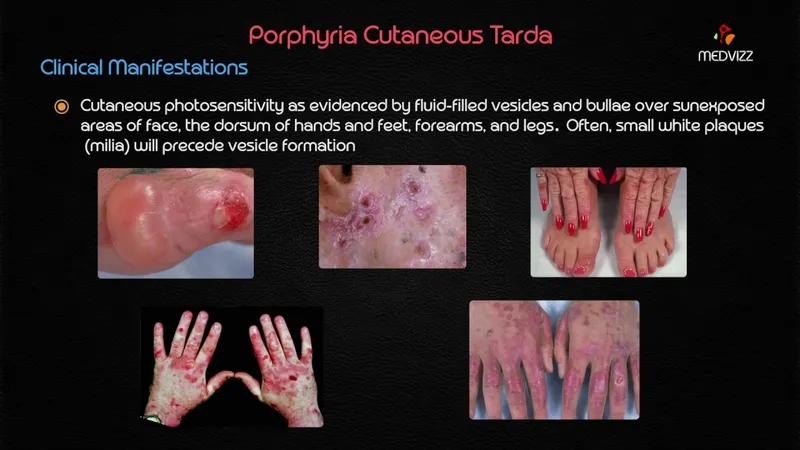
- It is caused by a deficiency in **uroporphyrinogen decarboxylase (UROD)**, leading to photosensitivity due to accumulated porphyrins in the skin.
*Hereditary Coproporphyria*
- This is an **autosomal dominant** disorder caused by a deficiency in **coproporphyrinogen oxidase (CPOX)**.
- It can present with both neurovisceral attacks and photosensitivity, depending on the accumulated porphyrins.
Porphyrias Indian Medical PG Question 4: In G6PD deficiency, which enzyme's function is MOST directly impaired due to decreased NADPH availability, leading to reduced protection against oxidative stress?
- A. Catalase
- B. Pyruvate kinase
- C. Superoxide dismutase
- D. Glutathione reductase (Correct Answer)
Porphyrias Explanation: ***Glutathione reductase***
- **G6PD deficiency** impairs the production of **NADPH** through the pentose phosphate pathway
- **Glutathione reductase** is NADPH-dependent and reduces oxidized glutathione (GSSG) back to reduced glutathione (GSH)
- Without adequate NADPH, glutathione reductase cannot maintain sufficient **GSH levels**, which is the primary antioxidant protecting RBCs from oxidative damage
- This explains why G6PD deficiency leads to **hemolysis** when exposed to oxidative stressors (antimalarials, sulfonamides, fava beans)
*Catalase*
- **Catalase** decomposes hydrogen peroxide to water and oxygen, protecting cells from oxidative damage
- While important for antioxidant defense, catalase does **not require NADPH** for its function
- Its activity is not directly impaired by decreased NADPH in G6PD deficiency
*Pyruvate kinase*
- **Pyruvate kinase** catalyzes the final step of **glycolysis**, producing ATP
- Its function is **completely independent** of NADPH levels
- Pyruvate kinase deficiency causes a separate hemolytic anemia unrelated to oxidative stress or G6PD deficiency
*Superoxide dismutase*
- **Superoxide dismutase (SOD)** converts superoxide radicals to hydrogen peroxide and oxygen
- SOD functions **independently of NADPH** and uses metal cofactors (Cu/Zn or Mn)
- While part of antioxidant defense, it is not directly affected by G6PD deficiency
Porphyrias Indian Medical PG Question 5: A girl who developed abdominal pain and presented to the emergency department with a seizure after taking sulphonamides is likely to have a diagnosis of:
- A. Acute intermittent porphyria due to other triggers (Correct Answer)
- B. Congenital erythropoietic porphyria with skin manifestations
- C. Infectious mononucleosis with fever and lymphadenopathy
- D. Kawasaki disease with prolonged fever and rash
Porphyrias Explanation: ***Acute intermittent porphyria due to other triggers***
- The combination of **abdominal pain**, **seizure**, and the **ingestion of sulfonamides** (a known trigger) is highly suggestive of an acute porphyric attack [1].
- **Sulfonamides** induce δ-aminolevulinate synthase, leading to an overproduction of neurotoxic porphyrin precursors [1].
*Congenital erythropoietic porphyria with skin manifestations*
- This condition primarily presents with **severe photosensitivity**, **blistering skin lesions**, and **hemolytic anemia**, rather than acute neurological symptoms [1].
- While it is a type of porphyria, its clinical presentation and triggers are distinct from the neurovisceral symptoms described.
*Infectious mononucleosis with fever and lymphadenopathy*
- Characterized by **fever**, **fatigue**, **sore throat**, and **lymphadenopathy**, symptoms not aligned with the severe abdominal pain and seizure observed.
- This condition is caused by the Epstein-Barr virus and is not triggered by sulfonamide use.
*Kawasaki disease with prolonged fever and rash*
- This is an **acute vasculitis** in children, involving **prolonged fever**, **rash**, **conjunctivitis**, and lymphadenopathy, but not seizures or abdominal pain caused by sulfonamides.
- It primarily affects the cardiovascular system and is not related to porphyria or drug-induced attacks.
Porphyrias Indian Medical PG Question 6: Which of the following is not classified as a cutaneous porphyria?
- A. Congenital erythropoietic porphyria
- B. Erythropoietic protoporphyria
- C. Sideroblastic anemia (Correct Answer)
- D. Hereditary coproporphyria
Porphyrias Explanation: ***Hereditary coproporphyria***
- This condition is primarily associated with **acute episodes** and **neuropathy**, rather than cutaneous manifestations. [2]
- Unlike cutaneous porphyrias, symptoms are more systemic and do not commonly present with **skin lesions**. Although skin features can occur in some instances, they mimic porphyria cutanea tarda. [2]
*Congenital erythropoeitic porphyria*
- Characterized by severe **cutaneous symptoms** such as blistering and photosensitivity due to **skin exposure**.
- Patients exhibit notable **facial disfigurement** and can have **hemolytic anemia**, aligning it clearly with the cutaneous forms of porphyria.
*Sideroblastic anemia*
- This condition involves issues with **hemoglobin synthesis** and does not fit the porphyria classification. [1]
- It primarily presents with **microcytic anemia**, and the symptoms are primarily hematological, not cutaneous. [1]
*Erythropoeitic porphyria*
- Characterized by **severe photosensitivity** and skin manifestations, similar to congenital erythropoeitic porphyria. [1]
- Patients may develop **blisters** and **hyperpigmentation** upon sun exposure, categorizing it among cutaneous porphyrias. [2]
Porphyrias Indian Medical PG Question 7: Which of the following is NOT a characteristic feature of Henoch-Schönlein purpura (HSP)?
- A. Splinter hemorrhage
- B. Thrombocytopenia (Correct Answer)
- C. Abdominal pain
- D. Epistaxis
Porphyrias Explanation: ***Thrombocytopenia***
- **Thrombocytopenia** is generally **not a feature** of Henoch-Schönlein purpura (HSP); platelet counts are typically **normal** or can even be elevated [1].
- HSP is a **vasculitis**, characterized by **IgA deposition**, leading to palpable purpura, rather than a primary platelet disorder [1].
*Splinter hemorrhage*
- **Splinter hemorrhages** are a form of **microembolism** or capillary damage that can occur in various conditions, and while not a cardinal feature, they are more related to vessel damage than thrombocytopenia.
- Although less common, any form of **vasculitis-related capillary leakage** could theoretically lead to small hemorrhagic phenomena.
*Abdominal pain*
- **Abdominal pain** is a very common and significant symptom in HSP, often due to **gastrointestinal vasculitis** leading to bowel wall edema, hemorrhage, or intussusception.
- It can range from mild discomfort to severe, colicky pain and may be accompanied by **gastrointestinal bleeding**.
*Epistaxis*
- **Epistaxis** (nosebleeds) is a possible manifestation of **mucosal vasculitis** in HSP.
- It can occur due to damage to superficial blood vessels in the nasal passages as part of the systemic inflammatory process.
Porphyrias Indian Medical PG Question 8: Pruritus [Itching] associated with Congenital Erythropoietic Porphyria is caused by deficiency of -
- A. Uroporphyrinogen - III synthase (Correct Answer)
- B. Uroporphyrinogen - I synthase
- C. 5-ALA dehydratase
- D. HMB synthase
Porphyrias Explanation: ***Uroporphyrinogen - III synthase***
- Congenital Erythropoietic Porphyria (CEP) is caused by a **deficiency of uroporphyrinogen III synthase**, leading to the accumulation of uroporphyrinogen I and coproporphyrinogen I.
- These accumulated **Type I porphyrinogens** are non-functional in heme synthesis and are highly **photoreactive**, causing the characteristic photosensitivity and skin symptoms, including intense pruritus.
*5-ALA dehydratase*
- Deficiency of **5-ALA dehydratase** (also known as porphobilinogen synthase) is associated with **ALA dehydratase deficiency porphyria (ADP)**, a very rare acute hepatic porphyria.
- Symptoms primarily involve **neurovisceral attacks** and do not typically include pruritus or photosensitivity.
*Uroporphyrinogen - I synthase*
- **Uroporphyrinogen I synthase** is an outdated and incorrect term; the correct enzyme in the heme synthesis pathway is **hydroxymethylbilane synthase (HMB synthase)** or **porphobilinogen deaminase (PBG deaminase)**, which synthesizes HMB.
- Deficiency in HMB synthase leads to **acute intermittent porphyria (AIP)**, characterized by acute neurological attacks, not severe pruritus.
*HMB synthase*
- **HMB synthase** (hydroxymethylbilane synthase), also known as **porphobilinogen deaminase (PBG deaminase)**, is deficient in **acute intermittent porphyria (AIP)**.
- AIP is marked by intermittent neurological dysfunction and abdominal pain, with **no significant photosensitivity or pruritus**.
Porphyrias Indian Medical PG Question 9: All are involved in bilirubin metabolism except?
- A. Biliverdin reductase
- B. Heme oxygenase
- C. Glucuronyl transferase
- D. ALA synthase (Correct Answer)
Porphyrias Explanation: ***ALA synthase***
- **ALA synthase** is the enzyme responsible for the first committed step in **heme synthesis**, not bilirubin metabolism.
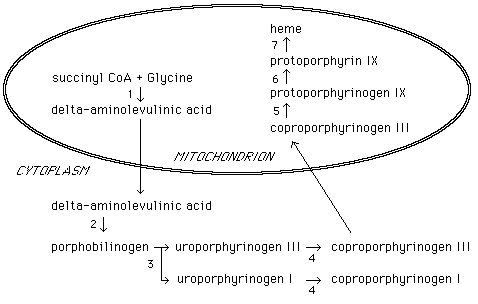
- It catalyzes the condensation of **succinyl CoA** and **glycine** to form δ-aminolevulinic acid (ALA).
*Biliverdin reductase*
- This enzyme catalyzes the conversion of **biliverdin**, a green pigment, into **unconjugated bilirubin**, a yellow pigment.
- It is an essential step in the breakdown pathway of **heme** into bilirubin.
*Heme oxygenase*
- **Heme oxygenase** is the enzyme that cleaves the **heme ring** to form **biliverdin**, releasing carbon monoxide and iron.
- This is the initial and rate-limiting step in **heme catabolism**, leading to bilirubin formation.
*Glucuronyl transferase*
- **UDP-glucuronyl transferase** (UGT) conjugates unconjugated bilirubin with **glucuronic acid** in the liver.
- This conjugation process makes bilirubin water-soluble, allowing its excretion into the **bile**.
Porphyrias Indian Medical PG Question 10: OATP 1B1/2 gene mutation is seen in which of the following conditions?
- A. Gilbert syndrome
- B. Rotor syndrome (Correct Answer)
- C. Crigler Najjar syndrome
- D. Dubin Johnson syndrome
Porphyrias Explanation: **Explanation:**
**Rotor Syndrome** is an autosomal recessive disorder characterized by chronic, conjugated (direct) hyperbilirubinemia. The molecular basis of this condition involves a **dual deficiency** of the hepatic uptake transporters **OATP1B1** and **OATP1B3** (encoded by the *SLCO1B1* and *SLCO1B3* genes). Under normal conditions, these transporters facilitate the re-uptake of conjugated bilirubin that has leaked into the sinusoidal blood back into the hepatocytes. When mutated, bilirubin cannot be re-absorbed, leading to elevated serum levels of conjugated bilirubin.
**Analysis of Incorrect Options:**
* **Gilbert Syndrome:** Caused by a mutation in the promoter region of the **UGT1A1** gene, leading to reduced activity of the bilirubin-glucuronosyltransferase enzyme. It results in mild, unconjugated hyperbilirubinemia.
* **Crigler-Najjar Syndrome:** Caused by severe mutations in the **UGT1A1** gene. Type I involves a total absence of the enzyme, while Type II involves a severe deficiency. Both result in significant unconjugated hyperbilirubinemia.
* **Dubin-Johnson Syndrome:** Caused by a mutation in the **MRP2** (ABCC2) gene, which encodes the canalicular multispecific organic anion transporter. This prevents the excretion of conjugated bilirubin into the bile, leading to a characteristic **black liver** due to melanin-like pigment accumulation.
**High-Yield Clinical Pearls for NEET-PG:**
* **Rotor vs. Dubin-Johnson:** In Rotor syndrome, the liver is **not** pigmented (normal appearance), and the total urinary coproporphyrin levels are elevated (with <70% being coproporphyrin I).
* **Oral Cholecystography:** The gallbladder is usually visualized in Rotor syndrome but **not** in Dubin-Johnson syndrome.
* **OATP1B1 Importance:** This transporter is also responsible for the hepatic uptake of **Statins**; mutations can increase the risk of statin-induced myopathy.
More Porphyrias Indian Medical PG questions available in the OnCourse app. Practice MCQs, flashcards, and get detailed explanations.